By Don Sadler
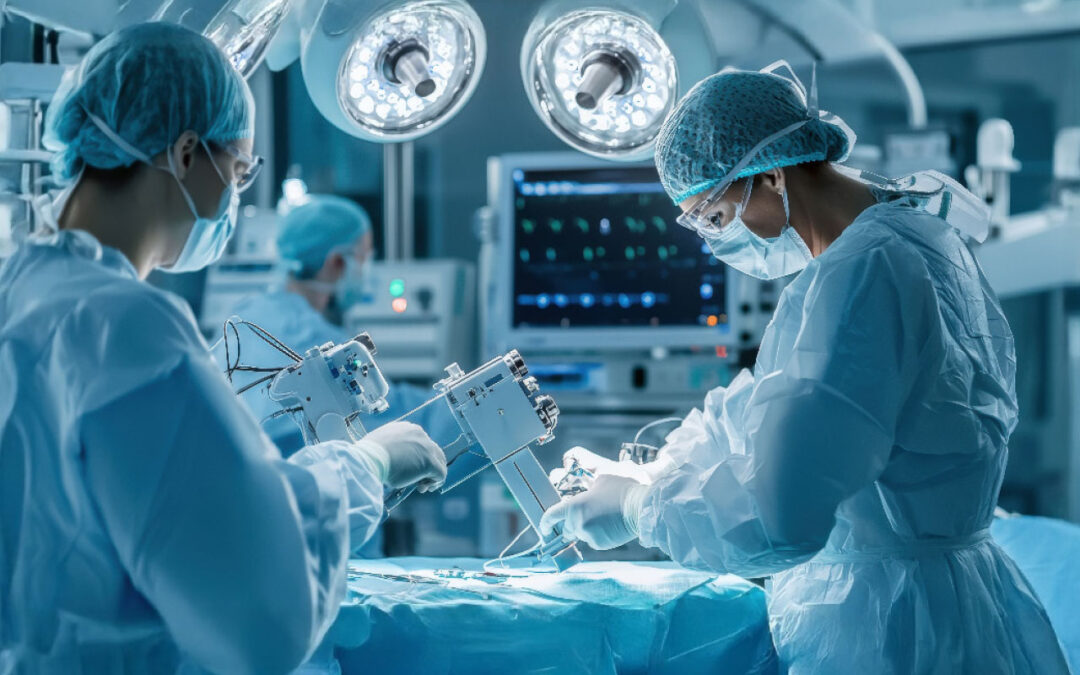
Technology is making major inroads in practically every industry today, including healthcare. Technological advances in operating rooms and ambulatory surgery centers are especially exciting.
Robotic surgical systems, hybrid operating rooms with real-time imaging, intraoperative image guidance, augmented reality (AR), the Internet of Medical Things (IoMT), OR Black Box recording, smart OR analytics and, of course, artificial intelligence (AI) are transforming ORs and ASCs into high-tech environments rivaling the most technologically advanced industries on the planet.
From Theoretical to Practical
According to orthopedic surgeon Evan D. Collins, MD, MBA, the innovator-in-residency for the Houston Methodist Center for Innovation, OR technology is moving from theoretical possibilities to practical probabilities.
“New technologies offer the potential to fundamentally change how patient care is delivered,” he says.
Collins lists artificial intelligence and ambient intelligence (AmI) as technologies that are being implemented across specialties to enhance the overall patient and provider experience.
“For example, we’re using AI to improve recognition of structures and tasks during an operation, which augments surgeon training,” he says.
“Other technology innovations are being deployed to improve OR efficiency and leverage better data processing technology to increase efficiencies and decrease waiting times for surgeries,” adds Collins.
By using AI, AmI and advanced systems to create more efficient, accurate and patient-centered processes, these technologies are addressing the growing demand for healthcare services while maintaining high quality patient care.
“However, we are steadfast in our view that AI and AmI function as a support system rather than a displacer,” says Collins. “For example, AI is excellent at processing large amounts of data and recognizing patterns, but the nuanced understanding of a patient’s individual needs can only come from a human clinician.”
Smart Hospital Optimizes AI
Houston Methodist Cypress Hospital opened in March as a “smart hospital” designed with some of the most advanced perioperative technologies available. It was built to optimize AI and human workforces to deliver more efficient patient care and improved outcomes.
“Houston Methodist is a hospital system rooted in innovation,” says Collins.
The hospital’s smart ORs feature ambient intelligence cameras that capture information about how cases are progressing and notify post-op team members about progress. These automatic alerts mean PACU doesn’t have to call the OR to find out when patients are headed their way. Family members are also updated on the patient’s status.
“Since we first launched ambient intelligence cameras in our ORs, we’ve been able to identify bottlenecks, gain real time insights and establish a culture of continuous improvement,” says Collins. “In addition, the technology has helped physicians optimize their time across multiple patients. Its success stems from consistent, transparent use and its ability to provide accurate, objective data that can drive process improvements.”
OR turnover time has improved by 16% since the hospital started using the ambient cameras, which has led to more than 1,500 additional cases. The efficiency gains allowed one surgeon to add a third case.
Houston Methodist Cypress Hospital is piloting the ambient camera technology with Apella.
“The technology helps predict and optimize surgical turnaround times, gain real-time insights and improve efficiency and accountability,” says Collins.
In addition, the hospital has implemented two-way cameras in patient rooms and deployed remote patient monitoring such as the BioButton, which offers continuous surveillance and early detection of changes in patient conditions.
“The ‘smart hospital’ concept isn’t always about having the most technology,” says Collins. “Rather, it’s about creating an adaptable infrastructure that can evolve with technological advancements.”

AI is a Game Changer
Tammy Hanks, DNP, APRN, PCNS-BC, NEA-BC, EBP-C, CNOR, Perioperative Practice Specialist with the Association of periOperative Registered Nurses (AORN), believes it’s hard to pinpoint the most impactful new technologies because it depends on what is needed for a specific patient population or specialty and whether the organization has the required infrastructure to support the new technology.
“As we all know, AI is a game-changer for perioperative nursing and has the potential to improve workflows and efficiency when leveraged appropriately,” says Hanks. “I believe almost all organizations can implement AI in some way that is meaningful for their staff and patient population.”
Hanks believes it’s also exciting to see how organizations and leaders are using smart OR analytics for scheduling, staffing and block utilization. “The OR Black Box Recording is another new technology with great potential to impact patient safety,” she says.
The biggest benefit of new OR technologies is their ability to improve patient safety and outcomes. “This should really be the driving force and common goal behind any new technology,” says Hanks.
There’s also the obvious competitive advantage for hospitals that comes with having the latest and greatest technology.
“Patients have many options when choosing where to have surgery,” says Hanks. “It does make a difference when organizations can tout not only new technology, but also its impact on patient outcomes and satisfaction.”
For perioperative teams, new OR technologies can play a big role in improving workflow, documentation and communication of critical intraoperative information while providing data and platforms for team training, education and clinical support.
“If organizations aren’t investing in new technology, they’re missing the opportunity to collect and leverage valuable data that can benefit the entire organization,” says Hanks.
Overcoming Staff Hesitation
Overcoming initial staff hesitation is a common challenge of implementing new OR technology.
“Hesitation may be due to fear of the unknown or a lack of confidence in their ability to master a new technology,” says Hanks. “Healthcare organizations and leaders are responsible for creating work environments where perioperative staff feel safe and trust that they are being heard and their concerns are being addressed.”
This includes listening to staff concerns and learning what hesitancies they have and why they are hesitant, which Hanks says is foundational to understanding how to promote change and the adoption of new technology.
“We need leaders who are committed to providing staff with comprehensive training and education on new technologies, verifying competency and identifying early adopters,” says Hanks. “We also need champions who can provide support to other staff members during the critical technology adoption time and clearly articulate how the new technology will positively impact staff and patients.”
Hanks believes that perioperative nurses should be included on the interdisciplinary team that evaluates and decides what new technology the organization should invest in.
“Their expertise and experience are vital to ensuring successful implementation of new technology,” she says. “Not only are they able to speak to the impact new technology will have on patients and workflow, but they will be crucial to ensuring staff buy-in during implementation.”
Collins believes that staff hesitation to adopt new technology is actually helpful in the long run.
“It’s not a problem to overcome, but rather a healthy part of the process,” he says. “Skepticism forces innovators to validate and prove new technologies, which ultimately benefits both patients and providers.”
With some new OR technologies, such as robotic surgery and hybrid ORs, the most important factor isn’t necessarily the technology itself but rather the surgeon’s level of expertise. “Innovative technology and techniques aren’t automatically better – you have to factor in the surgeon’s skill and experience,” says Collins.
Integrated AR-assisted Surgery
Vangie Dennis, MSN, RN, CNOR, CMLSO, FAORN, Partner, Perioperative Consulting LLC, believes that one of the most impactful new technologies introduced to the OR recently is AR-assisted surgery integrated with robotic platforms (e.g., da Vinci, Medtronic Hugo) and AI-based navigation systems (e.g., Medivis, Stryker’s AR systems).
“AR integrates with patient-specific 3D anatomy from CT/MRI scans and is directed to allow the surgeon’s view in real time,” Dennis explains.
This improves localization of tumors, nerves and vasculature; decreases the risk of damaging critical structures; and allows for more precision cuts, resections and implant placements.
This technology also improves anatomical accuracy by overlaying 3D reconstructions of the patient’s anatomy directly onto their body during surgery.
“Surgeons can see tumors, vessels, nerves or bones in real time without making large incisions,” says Dennis. “This reduces the risk of damaging critical structures and improves surgical accuracy.”
In spine surgery, for example, AR guidance has been shown to reduce pedicle screw misplacement rates compared to traditional methods.
AR is also a minimally invasive approach that allows surgeons to use smaller, targeted incisions.
“This lowers the risk of infections, blood loss, post-op pain and complications like hernias and adhesions,” says Dennis. “Patients also typically recover faster with fewer complications.”
There are also fewer imaging requirements since AR platforms can minimize intraoperative radiation exposure by reducing reliance on fluoroscopy (real-time X-rays).
“For example, in orthopedic and spine surgeries, preoperative CTs are fused with AR systems, which limits the need for repeated scans,” says Dennis.
AR-assisted surgery also reduces human error and allows faster and more confident decision-making. “Real-time data and AI-enhanced AR help surgeons quickly assess margins, angles or anomalies,” says Dennis.
The technology also enables immersive training for residents via simulation with real patient data, as well as remote assistance with specialists guiding surgeons in real-time via shared AR views. “This helps standardize care and improve outcomes in under-resourced settings,” says Dennis.
Using Robotics for TJRs
Last January, DISC Surgery Center in Newport Beach, California, introduced the use of a robotic arm to assist with total joint replacement (TJR) surgeries.
“Using robotic technology for total joint replacements has been going on for nearly a decade,” says OR Manager Justin Julian, who worked with OR nurse Christian Crothers to set up the technology. “We currently have two robots to assist with these procedures.”
According to Julian, using a robotic arm to assist with TJR surgery allows for improved accuracy of bone cuts and implant placement compared to traditional methods. “This is accomplished by taking a CT scan pre-operatively which is then used in surgery to create a 3D model of the patient’s joint,” he explains.
“During surgery, the robotic arm provides real-time feedback to surgeons, guiding them within the pre-defined boundaries of the surgical plan,” says Julian.
Through June, DISC Surgery Center had performed 131 robotic-assisted total joint replacement surgeries in 2025. This was nearly as many TJR surgeries (140) as were performed in all of 2024.
Technology to Prevent Hypodermic Needlestick Injuries
When Karen D. Orr, PA-C/CEO suffered a needlestick injury a few years ago and the patient had known Hepatitis C, she wondered why there wasn’t a product on the market to keep healthcare workers safe when using hypodermic needles.
“The good Lord gave me an idea for a new product that became HypoHolder,” says Orr.
After about three years of development, HypoHolder came to market in April.
“At first I sat on the idea because I didn’t know anything about entrepreneurship,” says Orr. “But no one was doing anything to keep us safe from needlestick injuries, so I asked a couple of friends to help me develop the idea into a product.”
HypoHolder is a safety engineered medical device that secures a hypodermic needle, allowing healthcare workers to uncap, recap and dispose of the hypodermic unit with just one hand. “At least 70 percent of hypodermic needlestick injuries occur during these three tasks,” says Orr.
Product evaluations with hospitals and ASCs started in July.
“The reactions have been amazing!” says Orr. “There’s an audible gasp or exclamation during demos as soon as I uncap a hypodermic needle with just one hand.” A few common reactions she hears: ‘That’s amazing!’ ‘Shut up!’ ‘Are you kidding me?’
Orr says she and her team are on a mission to stop hypodermic needlestick and other sharps injuries, which are up 16% from a decade ago, according to AORN.
“Healthcare is hard right now, so we want healthcare workers to know there are people who care about and appreciate them and the care they provide,” she says.
Embracing Technological Innovation
In his role as the innovator-in-residency at Houston Methodist’s Center for Innovation, Collins says it has been exciting to embrace technological innovation while maintaining a laser focus on patient outcomes and high-quality patient care.
“I’m optimistic about the future of healthcare technology, especially in the OR setting,” he says..