By Don Sadler
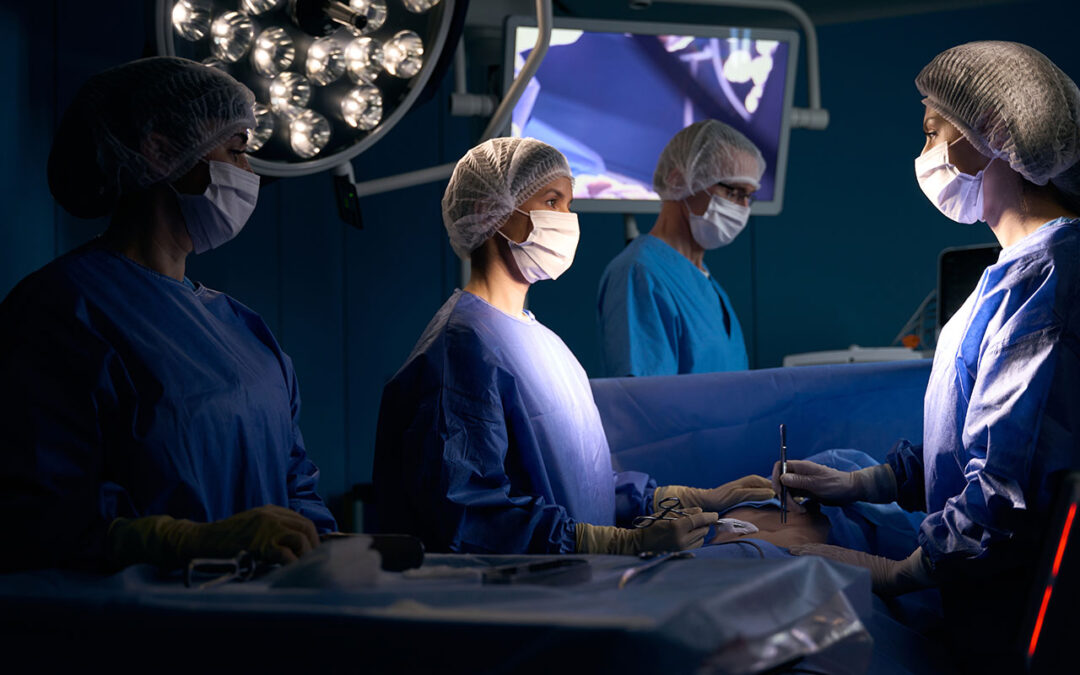
In a perfect world, every surgery would be performed risk-free. But such a world does not exist – and probably never will. Any time patients go under the knife, there’s a risk that complications could occur which result in negative patient outcomes.
The good news is that new technology tools are lowering the risk of surgical complications. These include robotic surgical systems, real-time imaging, intraoperative image guidance, smart OR analytics, augmented reality, machine learning, and artificial and ambient intelligence.
“AI and other advanced technologies can lower surgical risks by providing clinicians and institutions with the tools they need to improve risk predictions, surveillance and protocol adherence,” says Dr. Ido Zamberg, MD, MEHP, co-founder and chief medical officer at C8 Health, a best-practices implementation platform built specifically for healthcare teams.
For example, Zamberg cites a 2025 narrative review that determined AI-assisted robotic procedures were associated with a 30% decrease in intraoperative complications and a 25% reduction in operative time across multiple specialties.
Common Surgical Risks

Dr. Ido Zamberg, MD, MEHP, co-founder and chief medical officer at C8 Health
Among the most prevalent surgical risks are surgical site infections (SSIs), venous thromboembolism (VTE), surgical hemorrhage and adverse drug events (ADEs). “SSIs contribute significantly to morbidity, mortality and healthcare costs while VTE remains one of the most dangerous postoperative complications,” says Zamberg.
Zamberg notes a study that determined approximately one in 20 perioperative medication administrations result in a medication error or ADE, with more than a third causing patient harm.
According to Renae Wright, DNP, RN, CNOR, senior perioperative practice specialist, nursing practice with the Association of periOperative Registered Nurses (AORN), SSIs and VTE are best managed through infection prevention bundles and VTE prevention protocols. “There is no single intervention – reducing risk requires a multi-pronged approach,” she says.
“Improved infection control reduces SSI risk by ensuring that evidence-based prevention strategies are applied consistently, especially through the use of SSI prevention bundles,” adds Karen deKay, MSN, RN, EBP-C, CNOR, CIC, FAPIC, a senior perioperative practice specialist with AORN. “A systematic review determined that implementing care bundles led to fewer negative patient outcomes compared with using no bundle or only a single evidence-based practice.”
deKay notes statistics from the 2024 National and State Healthcare-Associated Infections Data Report indicating that while colon surgery SSIs decreased by 4% between 2023 and 2024, there was an 8% increase in abdominal hysterectomy SSIs.
“Because no single set of SSI‑prevention practices applies to all surgical procedures, prevention bundles must be continually evaluated and updated as new evidence emerges,” says deKay. “For perioperative nurses, staying current with evolving research and integrating recommendations across AORN guidelines is essential for minimizing SSI risk and supporting safe surgical outcomes.”
Beyond physiological and wound-specific effects, SSIs create a substantial clinical and economic burden. “Recent data further quantify this burden, showing the significant impact SSIs have on patient outcomes and healthcare resources,” says deKay.
For example, in a cross‑sectional propensity‑matched analysis of adult inpatients across 38 U.S. acute‑care hospitals, patients with SSIs required an additional 11.6 days of hospitalization and more than $30,000 in added hospital‑reported costs compared with matched controls without infection.
“The presence of SSIs also increased the risk of in‑hospital mortality more than threefold and raised the likelihood of hospital‑onset bacteremia more than sixfold,” says deKay.
Optimizing AI and Machine Learning

Tony DeDominico, vice president of operations at Houston Methodist
Houston Methodist Cypress Hospital opened last year as a “smart hospital” designed with some of the most advanced surgical technologies available to reduce surgical risk. It was built to optimize AI and human workforces to deliver improved surgical outcomes.
“Innovation lowers surgical risk by making care more precise, standardized and predictable across the perioperative journey,” says Tony DeDominico, vice president of operations at Houston Methodist. He cites the following technologies that can lower surgical risk:
- Minimally invasive and robotic-assisted surgery: These allow improved precision and control during complex procedures. Smaller incisions for appropriate patients result in less pain and blood loss, shorter hospital stays and faster recovery.
- Patient-facing digital pathways and education platforms: These permit mobile and text-based guidance across surgical episodes and step-by-step preparation and recovery instructions.
- Ambient intelligence, computer vision and automation: Embedded sensors, cameras and AI can unobtrusively capture real-time OR activity. In addition, automated real-time alerts keep surgeons, anesthesiologists and staff aligned without missed calls or pages.
- Remote monitoring and predictive analytics: These allow continuous physiologic monitoring beyond the OR, which can result in early detection of patient deterioration and faster intervention and escalation of care. “Additionally, they further extend safety through a virtual ICU model that monitors hundreds of beds, identifies risk earlier and provides additional support to frontline teams,” says DeDominico.
Houston Methodist also continues to expand ambient AI documentation, voice-enabled tools that support hands-free workflows in high-acuity environments, and experience-focused concepts such as virtual reality waiting room pilots.
Zamberg lists a number of specific ways that advanced technologies such as AI and machine learning can help lower surgical risks:
- Preoperative risk stratification: Machine learning models trained on routine perioperative variables such as demographics, comorbidities and procedure type are demonstrating strong predictive accuracy for postoperative complications including mortality, VTE and major bleeding.
- Intraoperative monitoring: AI and advanced monitoring technologies can analyze EEG signals to provide depth of anesthesia titration, reduce episodes of over- or under-sedation and personalize anesthetic dosing in real time.
- AI clinical decision support (CDS): AI-driven medication reconciliation tools and CDS systems have the potential to rapidly and accurately cross-check current medications, allergies, lab values and guidelines to flag high-risk combinations or dose errors before they are administered.
- Preventing “never events”: Computer vision and barcode or RFID systems are being piloted to verify implants, count sponges and instruments, and cross-check patient identity and procedure information in real time to help prevent RSIs and wrong-site/wrong-procedure surgeries.
“The value of these technologies is achieved through effective implementation,” says Zamberg. “Pushing best practices alongside clear ownership and institution-specific guidance can support clinicians and measurably reduce risk.”
“When patients feel informed and care teams share a common, accurate view of what is happening and what is coming next, risks can be anticipated earlier and addressed proactively instead of reactively,” adds DeDominico.
Human Experience and System-level Risks

Dr. Mark Sutton, vice chairman of the Houston Methodist Department of Urology
According to Dr. Mark Sutton, vice chairman of the Houston Methodist Department of Urology and the site director at the Houston Metro Urology Ambulatory Surgery Site for the Houston Methodist Urology Residency, surgical risk extends beyond clinical complications to include human experience and system-level risks. These include fear of the unknown, lack of control and breakdowns in coordination during a complex episode of care.
“In addition to well-recognized clinical risks such as infection, bleeding, pain, anesthesia-related side effects and blood clots, operational inefficiencies can significantly affect patient safety and surgical outcomes,” says Sutton. “When information is incomplete or inaccurate – such as imprecise documentation of start times, turnovers or preparation milestones – delays can compound across the surgical day.”
Houston Methodist has documented that even small discrepancies in documentation or communication can cascade into delays, overtime, unused OR time and increased risk for patients. “Innovation helps reduce these risks by improving clarity, communication and real-time visibility across the care journey,” says DeDominico.
Ambient intelligence is one solution the hospital is using to reduce operational inefficiencies. Using ceiling-mounted cameras, audio sensors and AI-driven computer vision, the system captures objective data across the surgical workflow, from preparation through turnover and cleaning. “This allows teams to receive real-time alerts, anticipate delays and maintain smoother surgical flow throughout the day,” says DeDominico.
Early returns have been impressive: The hospital has experienced a 43% improvement in on-time, first-case starts; a 20% decrease in turnover times; and a 15% increase in surgical cases without added staff or space.
After the surgery, hospital leaders can review aggregated workflow data to identify bottlenecks and improve processes. For example, did anesthesia setup slow things down? Was the patient prep time too long? Did room cleaning take longer than expected?
“It’s not about dissecting minute by minute or second by second,” says DeDominico. “It’s about looking at the overall flow of the room and figuring out where we can improve.”
Sterile Processing Technology Upgrades

Angie Thomas, Gritman Medical Center Surgery Director
Gritman Medical Center in Moscow, Idaho, recently completed a technology upgrade to its sterile processing department designed to enhance services and reduce surgical risk. These changes, which comply with the ANSI/AAMI ST108 guidelines, mandate utility water requirements for initial cleaning, critical water for final rinse and steam requirements utilized in sterilization.
“Water quality plays a key role that minimizes corrosion, pitting and scaling on instruments,” says Gritman Medical Center Surgery Director Angie Thomas. “In addition, water impurities can also decrease the effectiveness of detergents to clean instruments, which can increase a patient’s risk of infection and toxicity.”
According to Thomas, the new water management system minimizes stagnant areas of water within the distribution loops and provides continuous recirculation of water through UV light treatment and endotoxin filters.
Gritman Medical Center’s new sterile processing department also utilizes an electronic instrument tracking system. “This will further support and provide staff additional resources and tools that will help minimize human error factors and provide additional reinforcements and tools to provide compliance and oversight of regulatory standards,” says Thomas.
In addition, the sterile processing department added a cart washer to clean and wash all instrument pans and transport carts after each use. “This minimizes manual cleaning tactics and utilizes the same requirements and standards for instruments, containers and carts that transport instruments and supplies for each surgical procedure,” says Thomas.
Importance of Staff Well-Being

Cynthia Long, RN, PhD
One commonly overlooked factor in managing surgical risk is the well-being of the perioperative team.
“Working in the operating room demands intense concentration and sustained focus. There is no margin for distraction,” says end of life and grief coach Cynthia Long, RN, PhD. “When team members are fatigued, stressed, distracted or emotionally depleted, the risk of surgical error increases.”
For example, surgical staff could mix medications incorrectly, pass the wrong instrument, fail to notify PACU before transport or forget to apply the grounding pad for electrosurgery.
“The OR requires cognitive sharpness, emotional stability and physical stamina,” says Long. “Staff well-being is not a luxury – it is a patient safety strategy.”
Long lists several surgical risks that emerge when perioperative staff well-being is poor:
- Increased fatigue
- Decreased vigilance
- Slower reaction times
- Impaired communication
- Higher likelihood of near-miss events
- Increased burnout
“Burnout can lead to task-oriented behavior instead of mindful, patient-centered care,” says Long. “In surgery, where coordination and anticipation are critical, disengagement can compromise outcomes. A distracted mind in the OR can become a dangerous variable.”
Surgical leadership plays a critical role in reducing surgical risk due to poor staff well-being. Long offers a few suggestions for improving the well-being of OR staff:
- Conduct informative meetings to educate staff about new equipment, supplies and processes before implementation. “Clear communication reduces anxiety and prevents errors caused by unfamiliarity,” says Long.
- Protect staff relief breaks and mealtimes to minimize cognitive fatigue and improve concentration and performance.
- Create quiet or restoration zones. “One hospital I worked in provided a quiet room for rest and decompression and another offered a gym and exercise classes for staff,” says Long. “Having accessible spaces for physical and mental reset makes a measurable difference in staff well-being.”
- Offer special considerations for older, more experienced nurses. For example, Long notes a hospital that gave nurses over 55 years of age the option of no call during the week but only on holidays. “This recognition of the physical and emotional challenges older nurses face can help prevent burnout and support long-term engagement,” she says.
- Offer incentives for wellness, exercise and healthy eating. “When staff feel physically stronger, emotionally supported, and socially connected, they bring their best selves into the operating room,” says Long.
She recalled one hospital that provided Fitbits so employees could track their steps and earn gift cards as part of a wellness competition.
Long believes that patient safety begins not with the incision, but with the well-being of the team member holding the scalpel. “When we care for the caregivers, we reduce errors, improve communication and strengthen surgical outcomes,” she says.