Results show that first-of-its-kind device has a sustained treatment effect and a positive impact on quality of life
Royal Philips has announced positive two-year results from the Tack Optimized Balloon Angioplasty (TOBA) II below-the-knee (BTK) clinical trial. The data show the Philips Tack Endovascular System (4F), a first-of-its kind dissection repair device, provides a sustained treatment effect and positive impact on quality of life for Peripheral Artery Disease (PAD) and Critical Limb Ischemia (CLI) patients at two years. The data was presented by Co-Principal Investigator George Adams, MD, Interventional Cardiologist at Rex Hospital affiliated with the University of North Carolina at Chapel Hill, at the 2021 New Cardiovascular Horizons (NCVH) conference (June 1-4).
Across all patients in the TOBA II BTK clinical trial at two years, 73.6% had freedom from clinically driven target lesion revascularization (CD-TLR) and did not require a repeat procedure for the treated artery segment. CD-TLR is a commonly used indicator of treatment efficacy durability. In the more complex CLI patient population, which is typically associated with high rates of amputation and mortality, the data showed 94.7% target limb salvage (freedom from major amputation).
“The global endovascular community is diligently working to better understand how to restore blood flow in small limb vessels, promote healing and ultimately preserve limbs for people with CLI, one of the most vulnerable and critical patient populations,” said Dr. Adams. “These positive two-year data reiterate the clinical importance of below-the-knee dissection repair and validates the sustained durability of Tack-optimized interventions.”
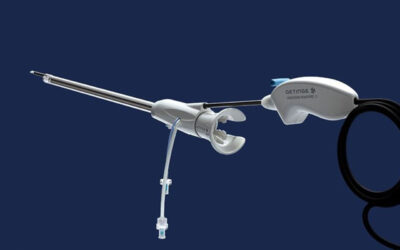
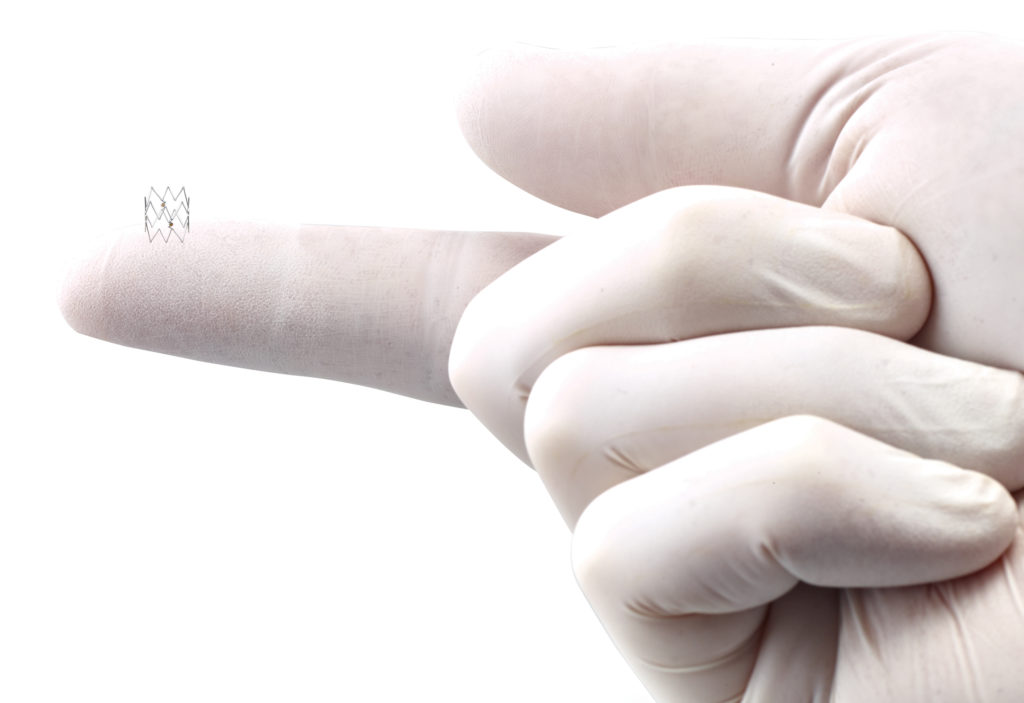
The Tack Endovascular System is a unique specialized implantable device to optimize the treatment of dissections in patients with PAD and its more advanced stage, CLI. CLI occurs when an obstruction in an artery severely reduces blood flow, causing painful wounds, debilitating rest pain, recurring ulcers and life-threatening infection. If left untreated, 50% of patients with CLI will undergo an amputation or die within the first year [1].
The two-year TOBA II BTK data also show sustained improvement in patients’ quality of life. In a patient questionnaire that assesses activity, pain and overall health, patients report having more control of their health and increased improvement in mobility.
“This new data further demonstrates the value of the Tack Endovascular System for repairing dissections and optimizing post-angioplasty outcomes in a challenging patient population,” said Chris Landon, Senior Vice President and General Manager, Image Guided Therapy Devices at Philips. “Dissection repair following balloon angioplasty has a positive, long-term value for both clinicians and patients alike. The implant is an important part of our complete procedural solutions to improve existing procedures and expand treatment options for PAD and CLI patients.”
The Tack Endovascular System is a first-of-its kind dissection repair device that is purpose-built to provide precision treatment of peripheral arterial dissections following balloon angioplasty in either above- or below-the-knee therapeutic interventions. The minimal-metal implant is designed to minimize vessel inflammation, promote healing, improve outcomes, preserve future treatment options for PAD and CLI patients and – ultimately – limbs. The Tack Endovascular System (4F) is the only vascular implant to receive U.S. Food and Drug (FDA) pre-market approval for BTK interventions, and TOBA II BTK is the first BTK investigational device exemption (IDE) study to enroll 100% dissected vessels.
The Tack Endovascular System is the most recent addition to Philips’ market-leading peripheral vascular portfolio, which includes advanced interventional imaging systems for precision guidance including Vascular Suite on its Image Guided Therapy System – Azurion; intravascular ultrasound (IVUS) catheters to assess the location of the disease and lesion morphology and guide and confirm the treatment; peripheral atherectomy devices to remove blockages; and peripheral therapy devices, such as Philips’ drug-coated balloon – Stellarex – to treat lesions.
The Tack Endovascular System is currently available for sale in the U.S. and some EU countries. Further information, including safety information, is available here.
[1] Hirsh AT, Jaskal ZJ, Hertzer , et al. ACC/AHA 2005 guidelines for the management of patients with peripheral arterial disease (lower extremity, renal, mesenteric, and abdominal aortic): executive summary a collaborative report from the American Association for Vascular Surgery/Society for Vascular Surgery, Society for Cardiovascular Angiography and Interventions, Society for Vascular Medicine and Biology, Society of Interventional Radiology, and the ACC/AHA Task Force on Practice Guidelines (Writing Committee to Develop Guidelines for the Management of Patients With Peripheral Arterial Disease) endorsed by the American Association of Cardiovascular and Pulmonary Rehabilitation; National Heart, Lung, and Blood Institute; Society for Vascular Nursing; TransAtlantic Inter-Society Consensus; and Vascular Disease Foundation. J Am Coll Cardiol. 2006 Mar 21;113(11):e463-654.