Baxter International Inc. announced the publication of two new analyses of real-world data regarding the use of Floseal Hemostatic Matrix in spinal surgeries. The retrospective studies observed better clinical and resource use outcomes in cases with billed charges for Floseal, when compared to cases with charges for Floseal in addition to certain non-flowable hemostatic agents. The studies were highlighted alongside Baxter’s Advanced Surgery portfolio innovation at the North American Spine Society meeting being held September 26-29.
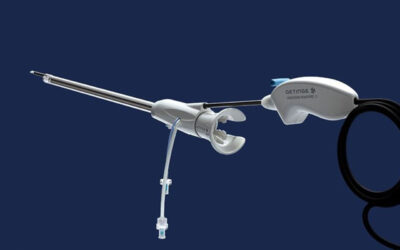
Addressing bleeding effectively and quickly during surgery is critical to avoiding major and minor complications for patients. Surgeons may use flowable hemostatic agents like Floseal in conjunction with non-flowable agents like gelatin sponges (Gelfoam) and thrombin when bleeding is not adequately controlled through suture, cautery, ligature or other conventional methods.
“This data suggests that the use of Floseal as a primary adjunctive hemostat during spine surgery correlates with measurable improvements for hospital administrators and surgeons such as length of stay and blood loss. This reinforces my belief that the choice of proper adjunctive hemostatic agent is a key component to driving down costs and complications for my patients,” said Nitin Khanna, M.D., minimally invasive orthopedic spine surgeon from Orthopedic Specialists of Northwest Indiana and co-author on the study published in Hospital Practice.
“Our retrospective analysis of a nationally representative hospital database observed favorable clinical and resource use outcomes in cases in which Floseal was the sole hemostat billed. While the inherent limitations of the study prevent us from assigning a causal relationship between Floseal-only use and improved outcomes, the real-world data nonetheless provide compelling support for the cost-effective use of Floseal from the start of intraoperative bleeding,” said Manuel G. Ramirez, M.D., MSc, the lead author on both publications and associate director of Health Economics and Outcomes Research for Baxter’s Advanced Surgery business.
In the first study published in Hospital Practice1, researchers studied retrospective data on 15,105 propensity-matched pairs of spinal surgeries from a large U.S. hospital billing database and found that cases with charges for Floseal, as the sole hemostat used in the case, were associated with 46 percent fewer blood transfusions and 38 percent lower blood-related complications than cases with charges for Floseal and other hemostats (gelatin sponges and thrombin).1 Floseal-only cases were also associated with nearly a half day shorter hospital stay, and 39-minute shorter surgical procedures.1 Limitations of the study included the retrospective database design and certain exceptions in the propensity score matching.
Researchers then developed a cost consequence model to calculate the potential cost savings associated with the improved clinical outcomes and lower resource use observed in the first study with the Floseal-only cases. The model concluded that the decreased resources, including shorter hospital stays and lower hemostat use, could potentially save medium volume U.S. hospitals $2,445 per spinal procedure.2 The results were published last month in the Journal of Medical Economics.
The studies include assessments of many cases with data extracted from Premier’s United States (U.S.) Perspective Database, which contains more than 490 million hospital encounters and captures approximately 25 percent of U.S. hospital discharges. Detailed explanations of the methodologies and study limitations are available in each respective publication.
Baxter shared the recently published data at the North American Spine Society annual meeting taking place this week in Los Angeles, Calif. Attendees can visit Baxter’s booth (#1915) to find out more about the studies and new enhancements coming soon to Floseal. Attendees can also learn more about the company’s expanding osteobiologics portfolio in the booth.
1 Manuel G. Ramirez, Harel Deutsch, Nitin Khanna, Donald Cheatem, Dongyan Yang & Erik Kuntze (2018) Floseal only versus in combination in spine surgery: a comparative, retrospective hospital database evaluation of clinical and healthcare resource outcomes, Hospital Practice, DOI: 10.1080/21548331.2018.1498279
2 Cost–consequence analysis of a hemostatic matrix alone or in combination for spine surgery patients. Manuel G. Ramirez, Xiaoli Niu, Josh Epstein & Dongyan Yang. Received 10 Jul 2017, Accepted 13 Aug 2018, Accepted author version posted online: 16 Aug 2018, Published online: 30 Aug 2018. https://doi.org/10.1080/13696998.2018.1513261