Forecast
Nurses are exiting the workforce and their facilities and quickly returning as patients. Hiring practices, retention efforts, and programs to ease the transition from school into practice are becoming a prime focus for hospitals.
1. Although many nurses are staying in the workforce longer than previously projected, there is still a demand for nurses, and this will continue to grow.
2. It is estimated that a facility loses $88,000 each time a nurse leaves a position and many are looking to do so soon.
3. The imminent retirement of the largest generation in modern history is creating a significant gap in the health care workforce and strain on facilities as they work to figure out how to adjust. One way to address this problem is easing new nurse transition and increasing nurse retention, identified by the Institute of Medicine in the milestone report “The Future of Nursing,” is the creation of nurse residency programs.
4. Experienced nurses are becoming a rare commodity but experienced perioperative nurses are even harder to find. In order to fill the vacancies, hospitals will need to grow their own.
Environment
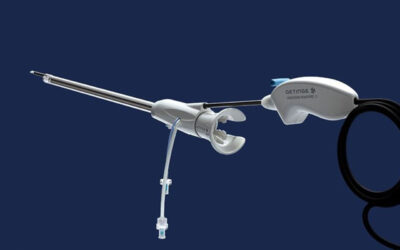
 New staff starting in the perioperative specialty have a huge learning curve, from the technical and fast paced envrionment to the complexity of case load.5 These challenges, paired with the high-tech nature of the equipment can seem titanic to the new nurse. If surgeries do not go as planned, the atmosphere in the operating room can become charged and intense, making it difficult for the new nurse to perform. A recent study showed that a one year residency offered the best opportunity for transition into practice for new graduate nurses.6 The perioperative nurse must be well trained and have the necessary support to navigate the many variables that may arise in the surgical setting.
New staff starting in the perioperative specialty have a huge learning curve, from the technical and fast paced envrionment to the complexity of case load.5 These challenges, paired with the high-tech nature of the equipment can seem titanic to the new nurse. If surgeries do not go as planned, the atmosphere in the operating room can become charged and intense, making it difficult for the new nurse to perform. A recent study showed that a one year residency offered the best opportunity for transition into practice for new graduate nurses.6 The perioperative nurse must be well trained and have the necessary support to navigate the many variables that may arise in the surgical setting.
Select the Seed
Just like picking a good strain of seed when planting a crop you want to make sure to select a candidate that has traits that align with the organization’s mission and values. Experience will be gained and skills can be taught, but behaviors, attitudes and values tend to be hardwired. A good way to predict the hardwired traits of a candidate is to utilize a standardized behavioral style interview process with an interdisciplinary panel. The most accurate predictor of future performance is often past performance in a similar situation.7 Panel members should consist of personnel within the department that have been instructed on the interviewing process and exhibit the traits you are looking for.
Churn the Soil
Once the resident has been selected, the soil must be prepared. Enrollment into a formal residency that has a foundation based on evidenced based practice (EBP) standards developed by the Association of periOperative Registered Nurses (AORN) will provide the necessary groundwork. The Periop 101: A Core CurriculumTM is a nationally recognized online program that sets the core requirements for a perioperative nurse’s education.
Nurse residents benefit from classroom time that uses case studies to promote critical thinking along with simulation labs that provide hands on opportunity. Historically learning retention rates from reading and lecture have been found to be as low as 20%, while open discussion and hands-on practice can improve learning retention up to 90% for the student.8 A microclimate of impressive knowledge can be transferred to the resident when classes are taught by experts in the field, such as surgeons, anesthesiologists, risk managers, perioperative leadership, and nurse educators to name a few. Face-to-face classroom time provides residents the freedom to debrief with peers, hear insightful stories, and ask questions about information presented. To promote professionalism and acquire experience with EBP, residents should be given time to investigate current practice on their units, using what they have learned about EBP in class. Evidence discovered can be communicated via a formal poster presentation to fellow residents as a cumulative project.
The final component that caps a residency program is a scrubbing rotation. The perioperative nurse who has never learned to scrub can be at a disadvantage when managing and coordinating the spectrum of intraoperative duties assigned to this role. The confidence to oversee and support activities at the sterile field is strengthened by the scrubbing experience.
Fertilize and Nurture
Residents must be given fertile soil, rich in knowledge and support, to foster the necessary growth and development to become a competent perioperative nurse. With formal training, preceptors and mentors can play significant roles in the development and success of a resident.
Preceptors share valuable stories and lessons learned that help guide the formation of sound clinical judgment for the resident. They must have strong communication skills, exhibit a willingness to be a preceptor, understand different learning styles, be effective at delivering constructive feedback, and display a positive supportive attitude. Preceptors help guide, teach, evaluate, shelter and advocate for the resident.5 It takes time for the resident to learn new tasks and become proficient in performing them. The resident and the preceptor must be partnered together, working in collaboration, and reinforcing what has been learned, until the resident feels confident and is deemed fully competent to work independently.
Mentors also play an important role in the resident’s development by providing professional and social support.5 They can help residents overcome common fears like making mistakes or not fitting in on a new unit. Mentors should exhibit professional demeanor, possess leadership skills, and be good at listening without passing judgment. Novice nurses gain confidence when mentors remain supportive and provide an objective perspective about issues the resident may be struggling with.5
Unit Culture
Many conditions may contribute to new graduate nurse turnover: abuse from fellow nurses, inadequate staffing that forces new nurses to be utilized as staff before finishing residency, and a culture that doesn’t adapt to change and continues to do things “like we’ve always done it.”9 The environment around the resident should be the product of a positive and healthy culture, a fair and just culture, one that is transparent and nurturing. The culture should embrace best practices and adapt EBP principles into the work done on the unit.9
Managers play a significant role in regulating the culture on a unit. Joint weekly meetings between the resident, preceptor and manager should take place.9 Meetings provide a formal time where goals can be created and assessed, room schedules and specialty rotations can be planned, and progress or potential problems can be identified and fixed.
Harvest
The old saying “you reap what you sow” has never been more relevant than when growing new nurses in the perioperative setting. If the organization is invested in the success of the resident, the harvest will be a success. If a crop does fail, an investigation should be done to identify all the possibilities that could have contributed to the failure, knowing that one person doesn’t have complete control over all the pieces. It takes dedication, collaboration, exploration and bravery to grow and retain valuable employees.
References
1. U.S. Bureau of Labor Statistics. Occupations with the Largest Projected Number of Job Openings Due to Growth and Replacement Needs, 2012 and Projected 2022. N.p., 2012. Web. 10 Oct. 2015.
2. “Nursing Shortage offset by Older Nurses Delaying Retirement” Culture of Health. Robert Wood Johnson Foundation, 8 Aug 2014. Web. 20 Oct. 2015.
3. Krsek, Cathy. “Investing in Nursing Retention Is a Smart Move in Today’s Economy.” American Nurse Today 6.4 (2011): n. pag. 2011. Web. 10 Oct. 2015.
4. The Future of Nursing: Leading Change, Advancing Health. Washington, D.C: National Academies Press, 2011. Print.
5. Persaud, Debra. “Mentoring the New Graduate Perioperative Nurse: A Valuable Retention Strategy.” AORN Journal 87.6 (2008): 1173-179. Web.
6. Kramer, M., Maguire, P., Halfer, D., Brewer, B., and Schmalenberg, C. “Impact of Residency Programs on Professional Socialization of Newly Licensed Registered Nurses.” Western Journal of Nursing Research 35.4 (2013): 459-96. Web.
7. Hansen, Katharine. “The Quintessential Guide to Behavioral Interviewing [Kindle Edition].” The Quintessential Guide to Behavioral Interviewing EBook: Katharine Hansen: Amazon.com.au: Kindle Store. N.p., 2012. Web. 10 Oct. 2015.
8. Dale, Edgar. Audiovisual Methods in Teaching. 3d ed. New York: Dryden, 1969. Print.
9. Duchscher, Judy and Myrick, Florence. “The Prevailing Winds of Oppression: Understanding the New Graduate Experience in Acute Care.” Nursing Forum 43.4 (2008): 191-206. Web.
Elizabeth Grigware, works in the Pacific Northwest for CHI Franciscan Health system. She is a Regional Perioperative Nurse Educator, with over ten years’ of accumulated experience in the perioperative setting.