By Don Sadler
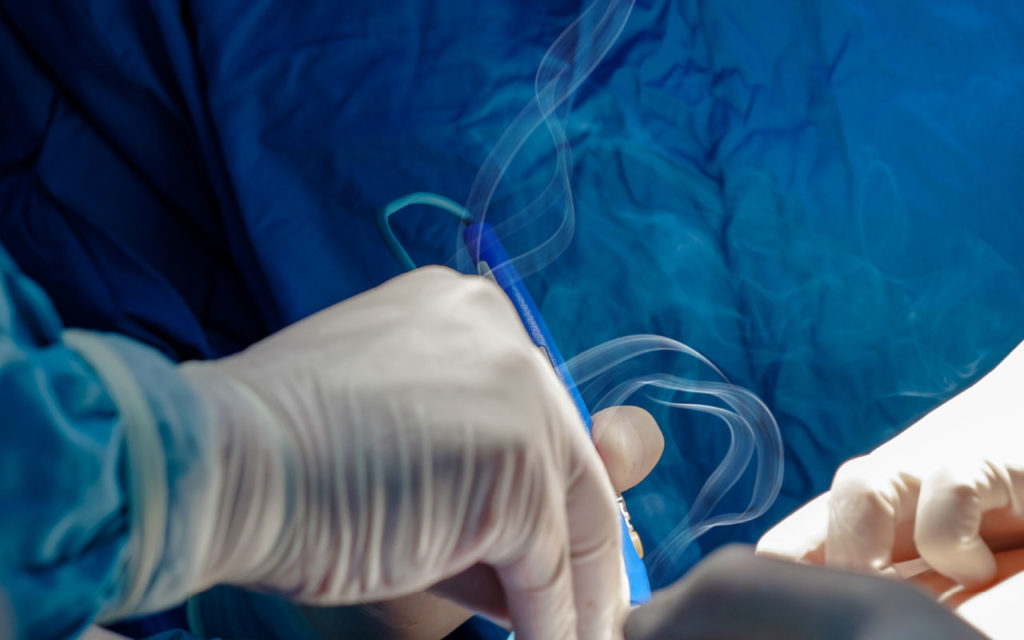
The dangers of surgical smoke in the operating room have long been apparent. Nearly four decades ago, it was first documented that particulate matter in surgical smoke can be inhaled and deposited in the lungs of OR personnel.
The health care profession has unfortunately been slow to deal with this problem. But this is finally starting to change: A growing number of states are introducing and passing legislation requiring hospitals and ambulatory surgery centers (ASCs) to use smoke evacuation systems to prevent human exposure to surgical smoke.
Three states have passed such legislation so far: Rhode Island, Colorado and, most recently, Kentucky, whose surgical smoke law passed in March of this year. In addition, surgical smoke legislation has been introduced in Connecticut, Georgia, Illinois, Iowa, New Jersey, Ohio, Oregon and Texas.
What is Surgical Smoke?
Surgical smoke is a byproduct created by the thermal destruction of tissue when using lasers, electrosurgical systems, radio frequency devices, hyfrecators, ultrasonic scalpels, power tools and other heat destructive devices in the OR, says Laura Gayton, MHCA, RN, CNOR, CSSM, associate director, standards interpretation for The Joint Commission.
“Research studies confirm that the surgical smoke plume can contain toxic gases and vapors such as benzene, hydrogen cyanide, formaldehyde, bioaerosols, dead and live cellular material (including blood fragments) and viruses,” says Gayton. “In some fields, it’s also possible to generate particulates and metal fumes.”
Gayton says that patient exposure to surgical smoke is short-term and relatively low risk. “However, surgeons, perioperative nurses and other OR staff are exposed to surgical smoke daily,” she says. “At high concentrations, the surgical smoke causes ocular and upper respiratory tract irritation and creates visual problems for the surgeon.”
“Most of what’s in surgical plume is 1.1 microns in size or smaller,” says Kay Ball, Ph.D, RN, CNOR, CMLSO, FAAN, a perioperative consultant and adjunct professor at Otterbein University in Westerville, Ohio.
“Any particles less than 10 microns can be irritating to lung tissue, and ultrafine particles can settle in alveoli, causing lung and air exchange problems,” says Ball. “Some of these particles may contain viable pathogens that can be transmitted in plume.”
Ball first performed research into the effects of surgical smoke on OR personnel in 2010 and then repeated parts of the research in 2020. “The results of the first study repeated 10 years later, which demonstrates a profile for perioperative nurses,” she says.
When asked if they had respiratory disorders or diseases, OR nurses in Ball’s study reported twice the incidences of respiratory problems compared to the general population. For example:
- 22.9% of OR nurses reported sinus infections and sinus problems compared to 11% of the general population
- 10.9% of OR nurses reported asthma compared to 7.6% of the general population
- 9% of OR nurses reported bronchitis compared to 3.4% in the general population
- 24.2% of OR nurses reported allergies compared to 15% in the general population
“There are many research studies that have shown the dangers of surgical smoke,” says Ball. “In AORN’s ‘Guideline for Surgical Smoke Safety,’ there are 223 references that help document the hazards of surgical smoke.”
In a study reported in the Journal of Clinical Nursing in 2016, 49% of nurses and 58% of surgeons reported experiencing headaches, 40% of nurses and 42% of surgeons reported watery eyes, and 49% of nurses and 28% of surgeons reported coughing due to exposure to surgical smoke.
Sore throat, nausea, drowsiness, dizziness, sneezing, rhinitis and bad odors absorbed in the hair were also attributed to surgical smoke by nurses and surgeons in this study.
Status of State Legislative Efforts
Brenda C. Ulmer, RN, MN, CNOR, has been spearheading efforts to get surgical smoke legislation passed in Georgia for more than two years. “Nurses and technicians who are tired of breathing smoke in the workplace are taking matters into their own hands by telling their story to legislators and asking for help through the political system,” she says.
Ulmer says she began her efforts after learning at the AORN Surgical Conference and Expo in 2019 that two states had passed surgical smoke laws.
“That’s when I decided Georgia should be the next state to pass legislation to protect patients and health care workers from surgical smoke,” says Ulmer, who was named the Georgia Council Legislative Chair in 2019. “It has been a seesaw journey since then.”
Due to the efforts of Ulmer and several others – including Vangie Dennis, MSN, RN, CNOR, CMLSO, assistant vice president, perioperative services with AnMed Health – two surgical smoke bills will be active on the first legislative day of 2022 in Georgia.
“Georgia is in a two-year legislative cycle so this puts us in a good position for getting legislation passed next year,” says Ulmer. “Georgia could be one of the next states to adopt surgical smoke legislation – hopefully by the spring of 2022, which is our goal.”
Unfortunately, surgical smoke legislation in Texas suffered a setback recently when legislation was pulled just before testimony was scheduled by Beverly Kirchner, president of the
Texas Collaboration of periOperative Registered Nurses (TCORN), and J.D. Buchert, MSN, M.Ed., MS, RN, president of the Dallas Association of Perioperative Nurses.
“We still have Senate Bill 429, but we were told that it would not make it to the committee this session,” says Kirchner. “We will now go the regulatory route instead of waiting 18 months to introduce the bill again. If we’re unsuccessful with the regulatory pathway, we will plan to come back and introduce the bill again in 2023.”
“As the president of TCORN, I plan to lead the effort to work with the Texas Health and Human Services and obtain a regulatory rule to ensure smoke evacuation is used to protect the perioperative team and the patient,” Kirchner adds.
Buchert points out that there is now four decades of knowledge and research when it comes to the dangers of surgical smoke. “With knowledge of people who have passed away and gone through cancer treatment due to inhaling surgical smoke, I believe our bill is important and needs to be passed to support the health of OR workers,” he says.
“My biggest reason for advocating so heavily on this topic is simple: Because it’s the right thing to do,” Buchert adds. “As perioperative nurses, we want to help save lives and not be put in danger while doing it.”
Ball says that her home state of Ohio introduced a smoke evacuation bill this spring. “The state bills are all very similar,” she says. “Most simply state that in hospital ORs or ambulatory surgery centers, a policy must exist on how to remove surgical smoke and the policy must be followed.”
Keys to Legislative Success
According to Jennifer Pennock, senior manager, government affairs, for the Association of periOperative Registered Nurses (AORN), surgical smoke evacuation legislation tends to be most successful in states with a strong group of grassroots advocates committed to working on policy advocacy for multiple years and through legislative sessions.
“To lay the groundwork for successful legislation, it is important for AORN and the advocates to engage with stakeholders early in the process,” says Pennock. “It’s also important to identify a strong bill sponsor in the House or Senate who will throw their political influence into the success of the bill.”
Support from state nurses’ associations and state hospital associations also contributes to the success of legislation, Pennock adds. “A strong bill sponsor can help all the stakeholders involved see the merits of the legislation,” she says.
Despite some setbacks and what might appear to be a slow pace, Ulmer believes that trying to get surgical smoke legislation passed at the state level is a smart strategy. “We have tried for many years to get some sort of national mandate on surgical smoke, but without success,” she says.
Often, the biggest obstacle to getting surgical smoke legislation passed by states is good old-fashioned politics.
“Georgia has been especially contentious with opposition from the hospital association and one particular surgeon,” says Ulmer. “Not to mention the political divide between Democrats and Republicans in the Georgia state legislature. We have learned as we’ve tried to work through the political system.”
In addition to legislation, there are also recommendations and guidance regarding surgical smoke from regulatory bodies. For example, NIOSH recommends that a smoke evacuator be on at all times when airborne particles are produced during all surgical or other procedures.
“Unfortunately, this is simply a recommendation and does not require compliance,” says Pennock.
“State laws requiring surgical smoke evacuation policies provide a pathway for the accrediting organizations to enforce facility adherence to their own policies on surgical smoke evacuation through the organization’s accreditation processes,” Pennock adds.
Steps to Reduce Surgical Smoke
It could obviously be quite some time before surgical smoke legislation is passed in all 50 states. So, what can hospitals and ASCs do in the meantime to reduce the risks of surgical smoke to OR personnel? Gayton recommends the following steps:
- Implement standard procedures for the removal of surgical smoke and plume through the use of engineering controls, such as smoke evacuators and high filtration masks.
“Use specific insufflators for patients undergoing laparoscopic procedures that lessen the accumulation of methemoglobin buildup in the intra-abdominal cavity,” says Gayton. “For example, a lapro-shield smoke evacuation device helps clear the field inside the abdomen.”
- During laser procedures, use standard precautions to prevent exposure to the aerosolized blood, blood byproducts and pathogens contained in surgical smoke plumes. “These include those promulgated by the Blood-Borne Pathogen Standard and the CDC’s Core Infection Prevention and Control Practices for Safe Healthcare Delivery in All Settings,” says Gayton.
- Establish and periodically review policies and procedures for surgical smoke safety and control. “Make these policies and procedures available to staff in all areas where surgical smoke is generated,” says Gayton.
- Provide surgical team members with initial and ongoing education and competency verification on surgical smoke safety, including the organization’s policies and procedures.
- Conduct periodic training exercises to assess surgical smoke precautions and consistent evacuation for the surgical suite or procedural area.
Gayton recommends reading The Joint Commission Quick Safety Issue 56 (http://tinyurl.com/4a7y937v) for more detailed guidance in alleviating the dangers of surgical smoke.
“Awareness of the dangers of surgical smoke has certainly increased when we consider the impact of The Joint Commission’s Quick Safety Alert, along with the growing interest in states to enact legislation,” says Pennock. “AORN also provides ongoing education about surgical smoke to our membership and the larger perioperative community.”
Pennock mentions the AORN Go Clear program specifically. “This is a comprehensive approach to protecting patient and worker safety by promoting a smoke-free environment wherever surgical smoke is generated,” she says. It includes all the tools and protocols needed to start or enhance smoke evacuation practices.
Since the AORN Go Clear program was first implemented, more than 1,200 facilities have registered for the program and 129 facilities have received the Go Clear award. “In addition, more than 19,000 facility staff are enrolled in the education portal,” says Pennock.
For more information about the AORN Go Clear program, visit https://www.aorn.org/member_apps/Product/Detail?productID=9709.










