Virginia Cancer Specialists, the largest private cancer practice in Northern Virginia, and an affiliate of The US Oncology Network, has announced one of its breast surgeons, David Weintritt, MD, known for his innovative surgical approaches, has been recognized for developing a protocol and leading a clinical study resulting in FDA approval for the use of indocyanine green (ICG) dye in lymphatic mapping during breast cancer surgery.
The protocol provides a more accurate method of lymphatic mapping during breast cancer surgery both in sentinel node mapping for early-stage breast cancer and a procedure called axillary reverse mapping with lymphovenous anastomosis during surgery for more advanced breast cancer that requires a removal of a larger number of lymph nodes. This procedure reduces patients’ risk of lymphedema from as high as 40% to as low as 5%.

Renowned Breast Surgeon at Virginia Cancer Specialists, David Weintritt, MD, Leads Clinical Study for New FDA-Approved Technology in Breast Cancer Surgery that Can Reduce Debilitating Lymphedema to as Low as 5%
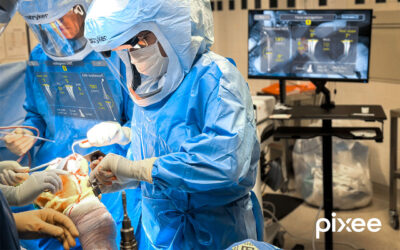
Weintritt saw an opportunity 7 or 8 years ago when evaluating a new camera system called SPY that allows operating surgeons to better visualize tissue perfusion during breast cancer reconstruction surgery. ICG, a drug that’s been proven safe and used for over 50 years, when injected and imaged with SPY, allows operating surgeons to “see” blood flow and detailed anatomy that would otherwise be invisible to the naked eye.
“Camera systems like SPY are used to visualize lymphatic channels and other important anatomy using fluorescence imaging in the near-infrared spectrum. This combination of an injectable dye and sophisticated imaging illuminates lymphatic structures that otherwise we wouldn’t be able to see, allowing surgeons to either avoid injuring them or have the ability to repair them during surgery,” shared Weintritt.
“I started researching all the reported applications of ICG in modern surgery and became aware of some anecdotal reports, mostly in literature outside of the US that alluded to ICG being used for mapping of the lymphatics for breast cancer surgery. However, the FDA had not evaluated or approved its use in the US and there was no clear protocol that was proven successful in comparison to other techniques,” shared Weintritt.
Weintritt then worked with the developers of the SPY camera on a standardized protocol for lymphatic mapping in breast cancer surgery.
Weintritt’s findings were then submitted to the FDA and the FILM B — Fluorescence Imaging and Lymphatic Mapping in Breast cancer surgery — study, which began in partnership with study sponsor Stryker. Together, with Weintritt at the helm as principal investigator, they launched the FILM B study and patients were enrolled across 7 sites in the US and Canada. The study findings were presented and gained FDA approval because the data showed this technique for lymphatic mapping and breast cancer surgery was equal to or better than the standard of care currently in use. The procedure offered 100 percent control to the operating surgeon and allowed for a better visualization of the lymphatic system during breast cancer surgery.
More about axillary reverse mapping and lymphedema prevention:
The FILM B study results and FDA approval puts the technique of ICG and SPY lymphatic mapping into the hands of more breast cancer surgeons. This improves the ability to see nearly invisible lymphatic channels during breast cancer surgery. If these channels are injured, then patients can develop lifelong lymphedema or swelling of their arm up to 40% of the time. Reverse axillary mapping with ICG and SPY provides the clearest way to see anatomy during surgery and this gives operating surgeons a better chance to either avoid injuring lymphatic channels or better seeing them and performing a procedure called lymphovenous anastomsosis (LVA). LVA can take as little as 20-30 minutes to perform and can significantly reduce lymphedema risk.
“With LVA we can help a group that had a lymphedema risk as high as 40% and lower that risk to as low as 5%, as this intraoperative imaging allows us to see things better than any other technology or technique,” says Weintritt.