
With the demand for respirators exceeding supply during the pandemic, many facilities are reusing single-use masks. It is a good thing then, that researchers continue to up their game when it comes to sterility assurance, as detailed in three recent articles in AAMI’s peer-reviewed journal, Biomedical Instrumentation and Technology (BI&T).
Dry Heat Decontaminates Surgical Masks and Single-Use Respirators
A research team based out of the microbiological quality and sterility assurance department at Johnson & Johnson have determined that dry heat processing is “an appropriate method for repeated single-use respirator and surgical mask decontamination.”
The researchers confirmed that exposing a used mask to 176°F (80°C) for two hours sufficiently reduces a wide spectrum of Mycobacterium species and clears the equipment for additional use over the course of a single hospital or laboratory shift. Interestingly, the effectiveness of this method was found to fall off around the 20th cycle, limiting how frequently a facility may choose to reuse masks.
Naturally, the researchers warn that soiled surgical masks and respirators are not fit for reuse.
“The dry heat process presented in this article should only be applied to visibly clean single-use respirators and surgical masks, with a focus on inactivating microorganisms remaining after use while preserving functionality,” the authors write.
Read more at: https://bit.ly/3cUqDne.

Important Definitions for Face Mask Processing
Reusing a mask that is, by definition, “single-use” can be confusing. Several of the J&J researchers who oversaw the dry heat experiments also set out to clarify key terms for sterility assurance departments during these unusual times.
In a review of academic literature and online commentary, the researchers outlined key definitions for “decontamination,” “disinfection” and “sterilization.” For instance, they highlight that “decontamination” has a slightly different definition in the U.S. verses how it is used internationally. Because of this, the researchers concluded that possible interpretations for “decontamination” may be too broad and, at times, may imply a level of clean that is impossible to achieve with common processing practices.
Taking things further, they highlight that “even low-level disinfection processes, defined as killing most vegetative bacteria, some viruses and some fungi would be considered effective against SARS-CoV-2.”
Thus, if the point of mask processing during the COVID-19 pandemic is to stop the spread of SARS-CoV-2, defining all effective cleaning processes as “disinfection” may help prevent confusion.
Read more at: https://bit.ly/3rARGrO.
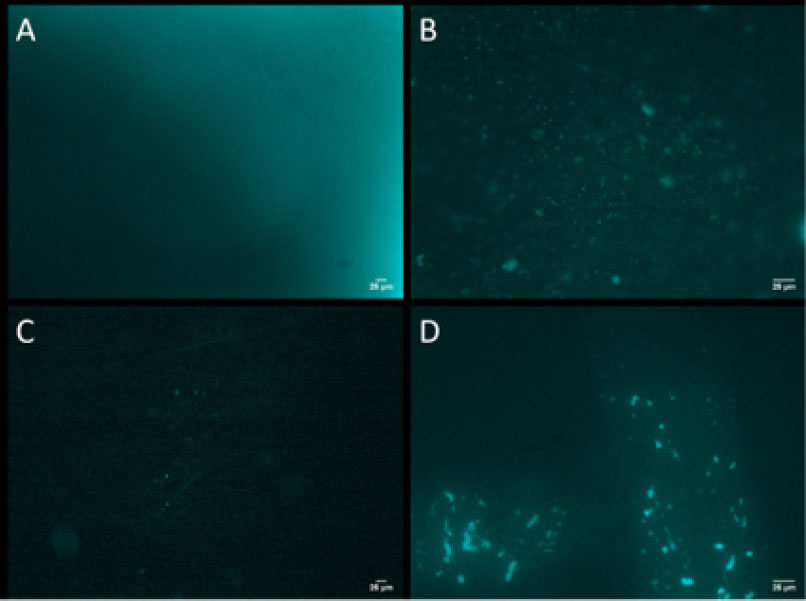
BAC-VIS with widefield and confocal fluorescence microscopy is used to observe bacterial cells on inoculated endoscope end cap material and O-rings. Panels A and C are controls.
Highlighting Potential Outbreak Sources
Even with hospitals focused on keeping the SARS-CoV-2 virus at bay, bacterial contamination remains a concern. Improper processing of endoscopes has been associated with several multi-patient outbreaks. That’s why a team of researchers from the Food and Drug Administration’s Center for Devices and Radiological Health and Healthmark Industries recently developed a new technique for visualizing where contamination may reside in a medical device even after being cleaned.
“Most published studies have focused on overall contamination rather than locating the sources and design features related to contamination,” the authors wrote. “Therefore, developing approaches for imaging bacteria on processed device parts is important.”
Their paper outlines a simple four-step protocol for a stain test that detects bacteria on endoscopes or scope parts. The BAC-VIS procedure allows for concentrations of bacteria remaining on a cleaned device to glow brightly for fluorescence imaging, showing researchers where contamination may occur. These results could help lead to better cleaning procedures, device design and other preventive action.
Read more at: https://bit.ly/3rhjAZO.










