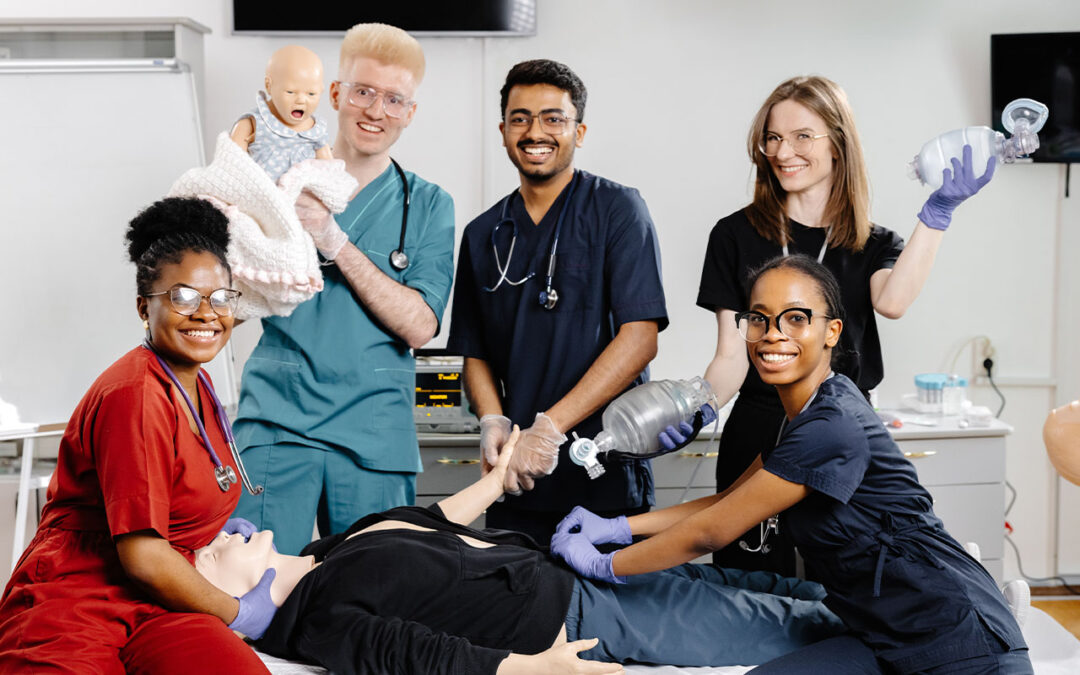
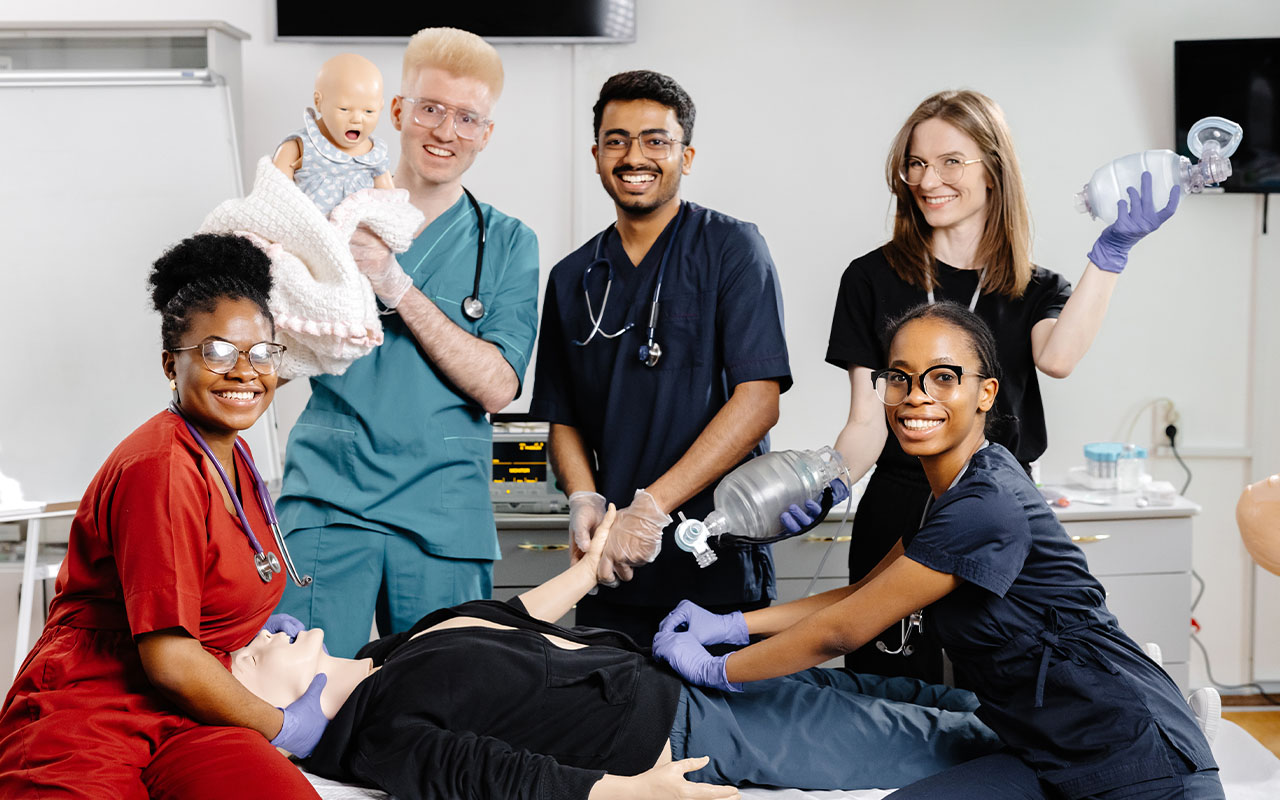
By Dawn Whiteside DNP, MSN, RN, CNOR, NPD-BC, RNFA
Nursing, recognized as the most trusted profession for 23 consecutive years, is projected to experience over 194,000 job openings annually through 2033 (AONL, n.d.; BLS, 2025). Within this landscape, perioperative nursing plays a critical role, impacting both clinical staff and leadership (Beitz, 2019). Despite its importance, the shortage of perioperative nurses has persisted for decades. Each year, approximately 46 million inpatient surgeries and 53 million outpatient procedures are performed in the United States (Beitz, 2019), underscoring the specialty’s centrality in healthcare.
Unfortunately, many nursing schools have reduced or eliminated exposure to perioperative nursing. A prevailing misconception – fueled by an overemphasis on standardized testing – is that perioperative nursing doesn’t utilize the nursing process and is therefore not “real” nursing. This view is not only inaccurate but detrimental. To counteract it, academic partnerships must emphasize the specialty’s clinical relevance and its alignment with core nursing competencies.
Historically, perioperative nursing was integrated into hospital-based diploma programs. When those programs phased out, so did much of the formal perioperative training. Today, more than 67% of nursing programs lack any perioperative content (Beitz, 2019). In response to the need for quality and safety-focused care, nursing schools collaborated to establish the Quality and Safety Education for Nurses (QSEN) initiative, which outlines six core competency domains: patient-centered care, teamwork and collaboration, evidence-based practice, quality improvement, safety, and informatics (QSEN, 2017).
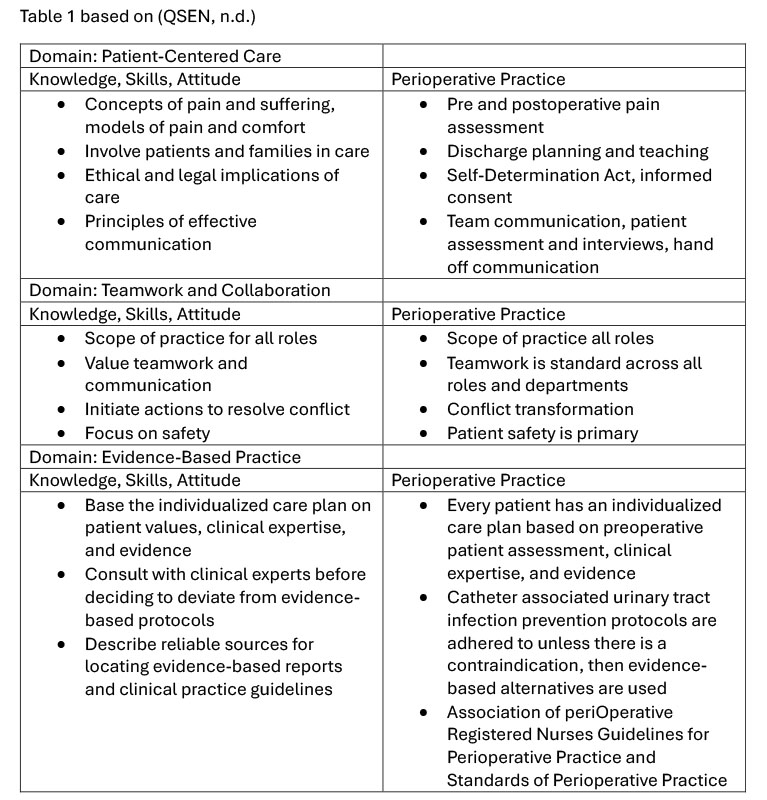
QSEN’s competencies mirror the skills needed in perioperative nursing. For instance, patient advocacy, teamwork, and safety protocols are foundational in both frameworks. Table 1 in the original source demonstrates the overlap between two QSEN domains and competencies central to perioperative practice. According to QSEN, preparing baccalaureate nurses for perioperative roles is critical. This preparation must integrate patient safety science, evidence-based care, and team collaboration (QSEN, 2017).
Baccalaureate nursing programs that exclude perioperative experiences are missing a valuable educational opportunity. Clinical exposure – whether through observation or elective rotations – offers nursing students hands-on experience in sterile technique, infection prevention, safety culture, advocacy, and systematic assessments (Beitz, 2019). These skills form a foundation for broader clinical competence. As Perron et al. (2020) note, new nurses must develop abilities in delegation, decision-making, conflict resolution, and constructive feedback – skills naturally fostered in the perioperative environment.
A promising model emerged in Houston, Texas, where a pilot program placed nursing students in the operating room at the start of their clinical education. While many nursing programs rely on lab and simulation for early clinical skills, this trial provided real-time, repeated exposure to activities such as sterile kit preparation, IV insertion, fluid administration, blood draws, and urinary catheterization (Tschirch et al., 2017). Students also gained valuable insights into mobility of patient transfers, team dynamics, and safety practice experiences that are difficult to replicate in other settings.
Residency programs, strongly recommended by the Institute of Medicine (IOM), are a key strategy in improving new nurse retention and clinical proficiency (Perron et al., 2020). While costly, residency programs save organizations money in the long run by reducing attrition and burnout. One innovative partnership between the Competency & Credentialing Institute (CCI) and Edgewood College in Madison, Wisconsin, has created a two-tiered, 16-week perioperative elective for prelicensure students. Graduates of this program are often hired directly into perioperative roles, with some facilities treating the elective as a residency equivalent. Several program alumni are now volunteering as mentors, helping to train the next cohort through perioperative “bootcamps” prior to clinical placements.
If the nursing profession is serious about addressing the ongoing shortage of perioperative nurses, innovative academic-clinical partnerships must become the norm. Introducing perioperative rotations early in a student’s clinical education not only reinforces fundamental nursing skills but also opens doors to a specialty too often overlooked. It’s time we invest in bold, practical solutions to secure the future of perioperative care.
References
- American Organization for Nursing Leadership (AONL), n.d. Gallup names nursing most trusted profession again. Retrieved May 6, 2025. https://www.aonl.org/news/Gallup-names-nursing-most-trusted-profession-again
- Beitz, J. M. (2019). The Perioperative Succession Crisis: A Cross-Sectional Study of Clinical Realities and Strategies for Academic Nursing. Nursing Economic$, 37(4), 179–197.
- Bureau of Labor Statistics (BLS), 2025. Occupational outlook handbook: Registered nurses. Retrieved May 6, 2025. https://www.bls.gov/ooh/healthcare/registered-nurses.htm#tab-6
- Perron, T., Gascoyne, M., Kallakavumkal, T., Kelly, M., & Demagistris, N. (2020). Effectiveness of Nurse Residency Programs. Journal of Nursing Practice Applications & Reviews of Research, 10(1), 48–52.
- Tschirch, P., Leyden, K., Dufrene, C. and Land, S. (2017), Introducing Perioperative Nursing as a Foundation for Clinical Practice. AORN Journal, 106: 121-127.
- Quality and Safety Education for Nurses. (2017). QSEN initiatives 2012. Clevland, OH; Author.
- Quality and Safety Education for Nurses. (n.d.). QSEN competencies. Retrieved May 6, 2025. https://www.qsen.org/competencies-pre-licensure-ksas
Table 1 based on (QSEN, n.d.)