Courtesy of Penn State Health
Mammograms remain the gold standard for detecting breast cancer in its earliest stages, potentially saving lives. So, why do some women receive a letter after a negative mammogram – meaning there’s no sign of cancer – asking them to consider additional tests?
The answer, according to Rebecca Sivarajah, M.D., a specialist in breast imaging with Penn State Health, boils down to the type of tissue in a woman’s breasts.
“Most breasts include both fatty tissue and the fibroglandular, or dense, tissue,” she said.
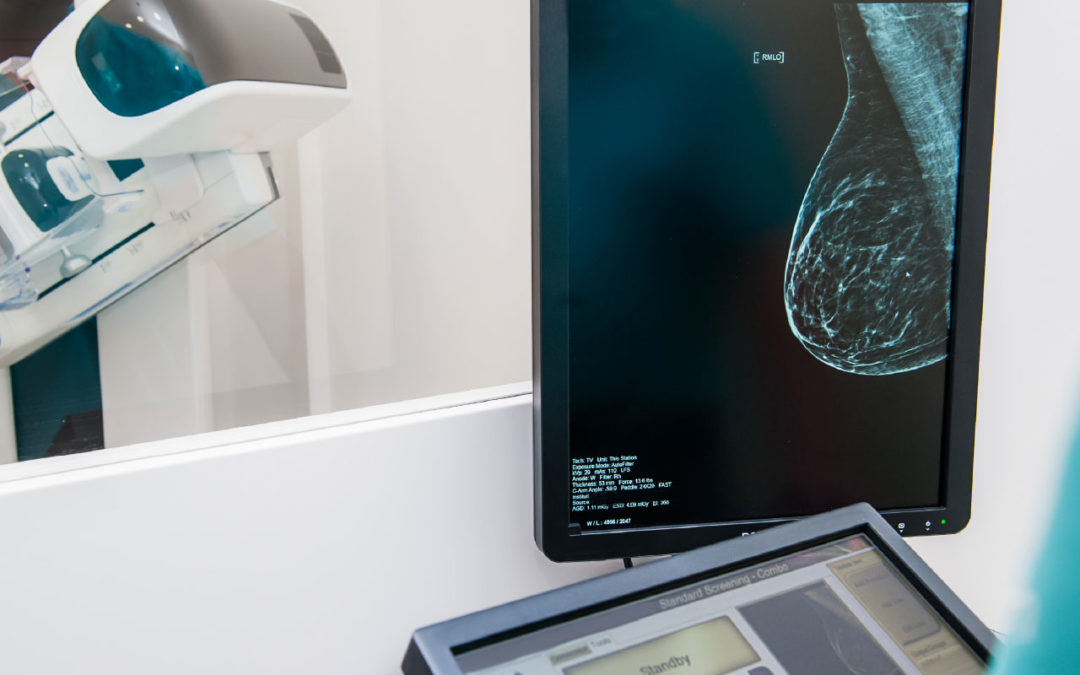
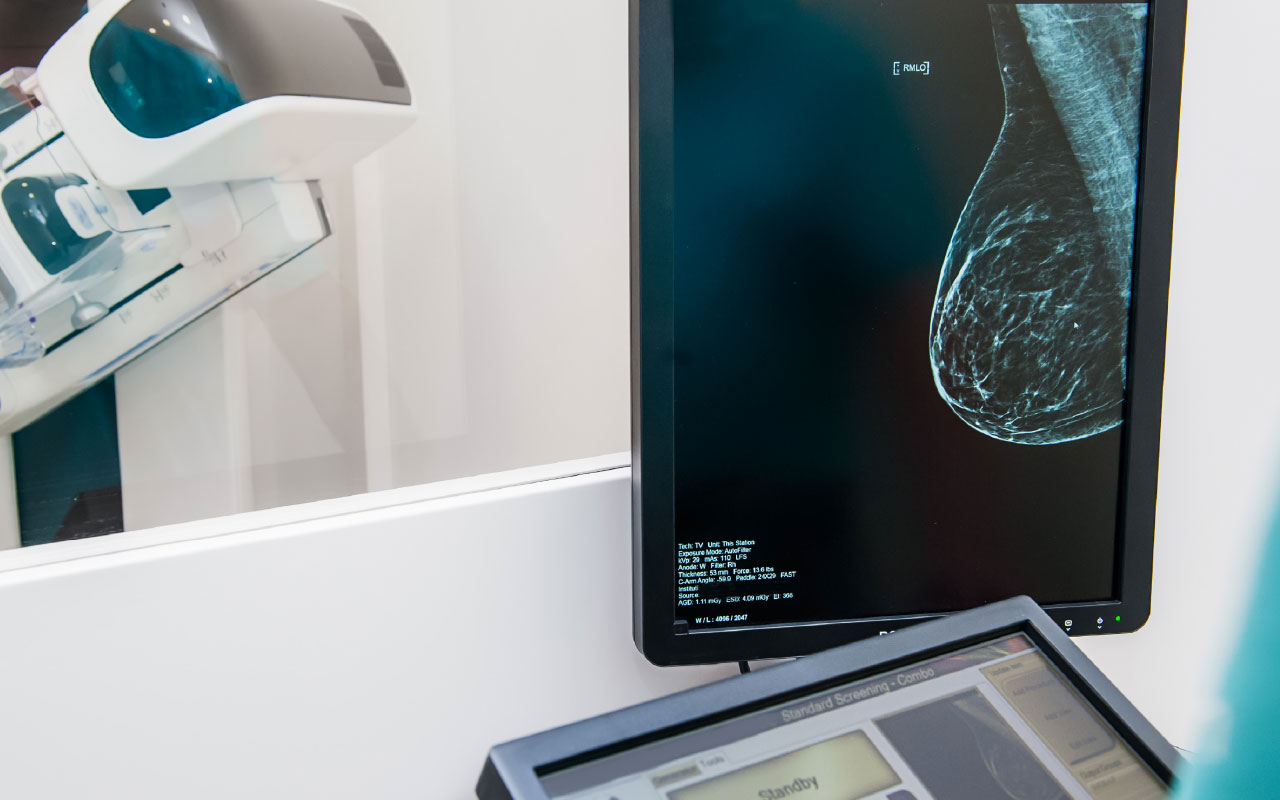
While fatty tissue appears grey on a mammogram, dense tissue appears white. Some cancer lesions also appear white on a mammogram.
“Therefore, high levels of dense tissue in some women may mask a cancer lesion on a mammogram,” Sivarajah said.
That’s why, six years ago, Pennsylvania enacted a law requiring radiologists to notify women with dense breast tissue about supplemental screenings following a negative mammogram. While the law raised awareness of the risks associated for women with dense breast tissue, the topic itself evokes many questions and myths.
Let’s separate some myths from the facts.
Myth 1: I can tell my breast density by the way they feel.
Fact: “In general, you can’t determine breast density by ‘feel,’ ” Sivarajah said. Instead, a mammogram will determine breast density. The American College of Radiology breaks down breast density into four classes. Women whose breasts rank in the “fatty” or “scattered fibroglandular tissue” classes do not have enough dense breast tissue to raise concern. Women whose breasts rank in the “heterogeneously dense” and “extremely dense” classes have high breast density. An estimated 40% of U.S. women fall into those latter two classes.
Myth 2: I can’t have dense breast tissue because I’m not overweight.
Fact: Obesity has little impact on breast density. “Being overweight or obese may increase the amount of fatty tissue in a woman’s breast, but it doesn’t increase the relative amount of dense breast tissue,” Sivarajah said. However, a woman’s breast density often decreases with age.
Myth 3: Breast density doesn’t affect my cancer risk.
Fact: “Women in the highest density class (‘extremely dense’) are more likely to be diagnosed with breast cancer compared to a woman in the lowest density class (‘fatty’),” Sivarajah said.
Myth 4: Because I have dense breasts, I don’t need a mammogram.
Fact: Supplemental tests do not take the place of a mammogram. “While dense breast tissue can make a mammogram less sensitive, mammograms can still find breast cancer,” Sivarajah said. In fact, some potential signs of breast cancer, such as certain calcifications and distortions, can only be found with a mammogram.
For most women with high breast density, a screening breast ultrasound is the most common supplemental test. Automated Breast Ultrasound Screening (ABUS) uses soundwaves – not radiation – to create a 3-D image of the breast. During this screening, a padded, curve-shaped transducer is placed on the breast while the patient lies down.
“The test is comfortable for most women,” Sivarajah says.
For women with a higher lifetime risk of cancer – 20% or more as determined by a doctor – breast MRI may be recommended as a supplemental test. This test uses magnets and contrast dye to enhance any potential lesions differently from dense breast tissue.
Most insurance plans cover ABUS or screening ultrasound of the breast. Breast MRI is often covered by insurance for patients who have an elevated lifetime risk greater than 20%. Patients should check with their insurance carrier to verify coverage.
So, what’s the best next step for women who get a letter about their breast density? “Talk with your primary care doctor about whether a supplemental test is right for you,” Sivarajah said.