By Matt Skoufalos
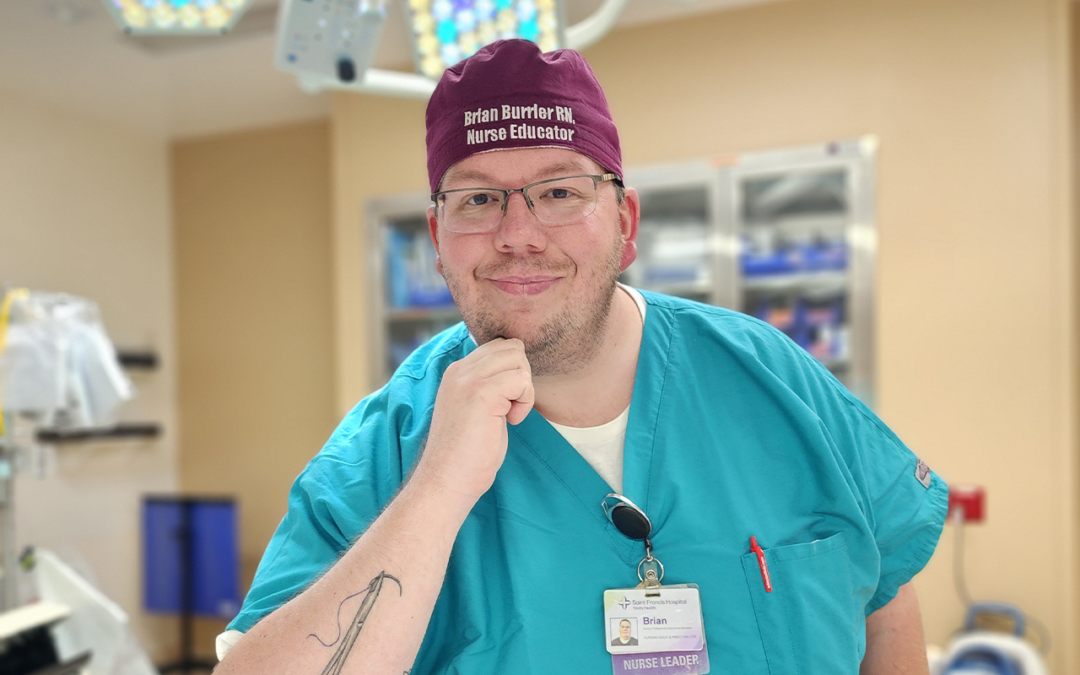
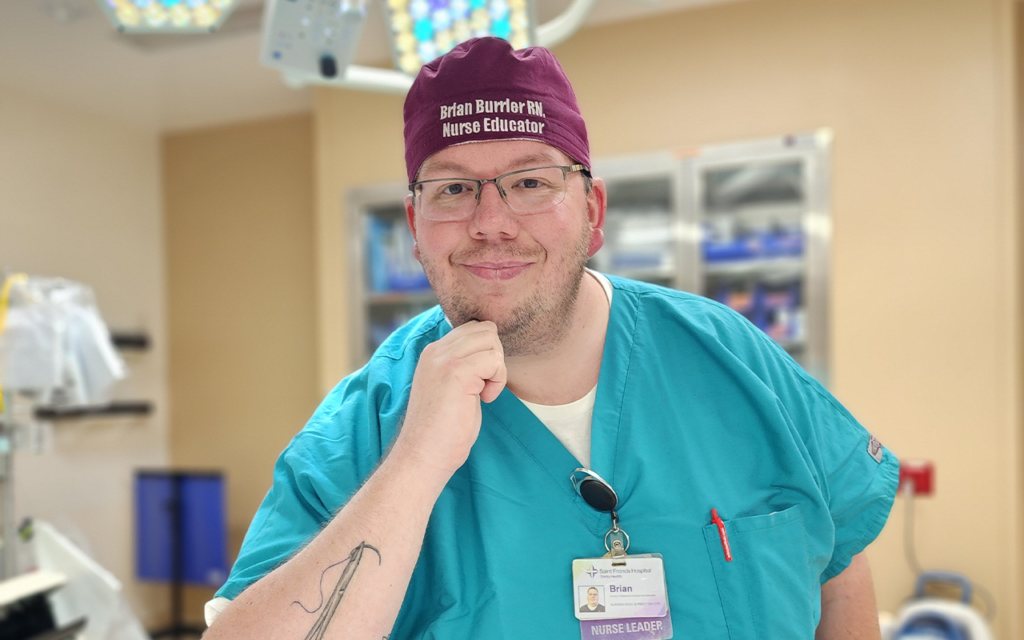
Brian Burrier comes from a long line of military service personnel. His parents met in the U.S. Army, and the family traveled frequently throughout his childhood. Burrier’s mother was a cook during her Army career, and he thought he might follow in her footsteps, taking up culinary arts at his technical high school in Connecticut. Burrier followed both his parents into the Army, also working as a cook; however, after his four-year term concluded, Burrier was less certain of his subsequent plans.
“I am extremely proud of my military service, and I would do it again in a heartbeat, but I was happy to have fulfilled my service,” Burrier said. “When I got out, I was lost as to what to do. Cooking is a passion of mine, but as a job, I wasn’t interested in it.”
Burrier enrolled in community college, and enjoyed chemistry classes enough that a friend’s mother, who was a nursing instructor at the school, suggested he might enjoy nursing. He was impressed by the variety of opportunities in the profession. When Burrier was finally given the opportunity to shadow an OR nurse, “it was a whole different world.
“My first time shadowing, I looked at the whole procedure, and when I left there, I was mesmerized,” he said. “I realized afterwards that I hadn’t spent much time focusing on what the nurse was doing in the OR. I asked if I could have a second rotation, and I really saw what the circulator did, and what the scrub nurse does, and I said, ‘This is it.’ ”
“When I was in Iraq, I had been a combat lifesaver,” Burrier said. “I had always had a passion for helping people, and I realized nursing similarly as a passion. I spent my second year of nursing just knowing I was going to be a perioperative nurse when I graduated. Imagine my surprise when I graduated in 2013 and it’s so hard to get into any specialty, especially the OR.”
At the time Burrier was preparing to enter the field, so many new nurse graduates were struggling to obtain even a medical-surgical appointment that he began sending his resume across the country in hopes of landing a bite in an OR setting. Of all the places to send an offer, the call came in from Bismarck, North Dakota asking whether Burrier could start in two weeks.

“I’d been traveling so much in the military that it was almost nothing for me to uproot my life,” he said. “I packed everything up, moved to North Dakota, and signed a two-year contract. It was a very challenging place to be, but I really took to it because I had that military spirit and discipline.”
Today, when Burrier leads a new nurse orientation, his charges complete it over a course of nine months of work. Back at the start of his career, his OR orientation was compressed into three months. When Burrier finally did get access to a Periop 101 class, the instruction came in the form of self-guided computer modules. Despite the limited training, Burrier had become the evening charge nurse by his second year in Bismarck, and eventually learned cardiac surgery as well. To avoid the bitter cold and lack of entertainment, he spent the winter months accelerating his schooling and completed a bachelor’s degree online in a little over a year.
From there, Burrier began working as a travel nurse, completing a master’s degree online while fulfilling nursing contracts in upstate New York and in specialty neurosurgery at Yale University in Connecticut. School was less of a struggle for him than was figuring out what to do with his master’s degree. Perioperative nursing doesn’t offer much upward mobility, and Burrier wasn’t really interested in a management track. Instead, he decided to pursue an educational degree so that he could specialize in an environment that facilitated his love of teaching.
Burier had received positive feedback on his work as a preceptor even during his travel nursing days, so when he began working as a nurse educator, he took the things that had worked for him in those environments and created a multimodal, six-week perioperative boot camp for new nurses entering the operating room environment. It includes a virtual library of video content mixed with scrub and gown classes, instrument classes, a suture class, and interactive simulations for a curriculum that touches on all kinds of learning styles.
“The OR is just so different than any form of nursing,” Burrier said. “When you think about all the different types of learning we have, some people learn better with lectures and modules, and some from watching the videos.”
“Sixty percent or more learn better with the hands-on kinesthetic approach,” he said. “You have to make it a multimodal experience for everybody. Traditionally they’d do the module, the video, and the hands-on positioning so they know what it feels like, but in procedural areas of nursing, it’s actually better to do the hands-on simulation education before they go through the didactic content.”
“Our surveys in the middle of classes showed they’d understand the content better if they had the hands-on before the computer module and the video,” Burrier said. “The only reason that works in the OR is because in nursing school, you’re already taught that didactic information already. By using the experiential learning theories, we can switch everything around, do the hands-on first, and then the module makes a whole lot more sense for them.”
Today, Burrier is a board member of the Connecticut chapter of the Association of periOperative Registered Nurses (AORN) who’s passionate about “trying to do larger things,” like bringing AORN events to his hospital, delivering nursing continuing education, and working with different vendors to get in-service trainings. Some of the education he’s helped to create at his current hospital “has gone system-wide,” Burrier said, including a unique sharps tray passing zone model that has resulted in a 50-percent drop in perioperative sharps injuries.
When Burrier isn’t at work, he enjoys hiking, cooking, and spending time with his two-year-old son. He’s very active in the Connecticut AORN chapter, leading community-based outreach, events, and educational dinners for chapter members. His wife, Frances, has her doctorate as a nurse practitioner with a mental health certification, and performs home-based primary care through the local VA hospital. Frances is a constant advocate for Burrier’s perioperative education career, and sees daily the passion he has for perioperative nursing.
Professional Spotlight Nomination