By Don Sadler
The healthcare industry is one of the biggest emitters of greenhouse gasses in the world. In fact, if healthcare were a nation, it would rank fifth globally in CO2 emissions. In the U.S., healthcare activities produce up to 10% of all greenhouse gasses.
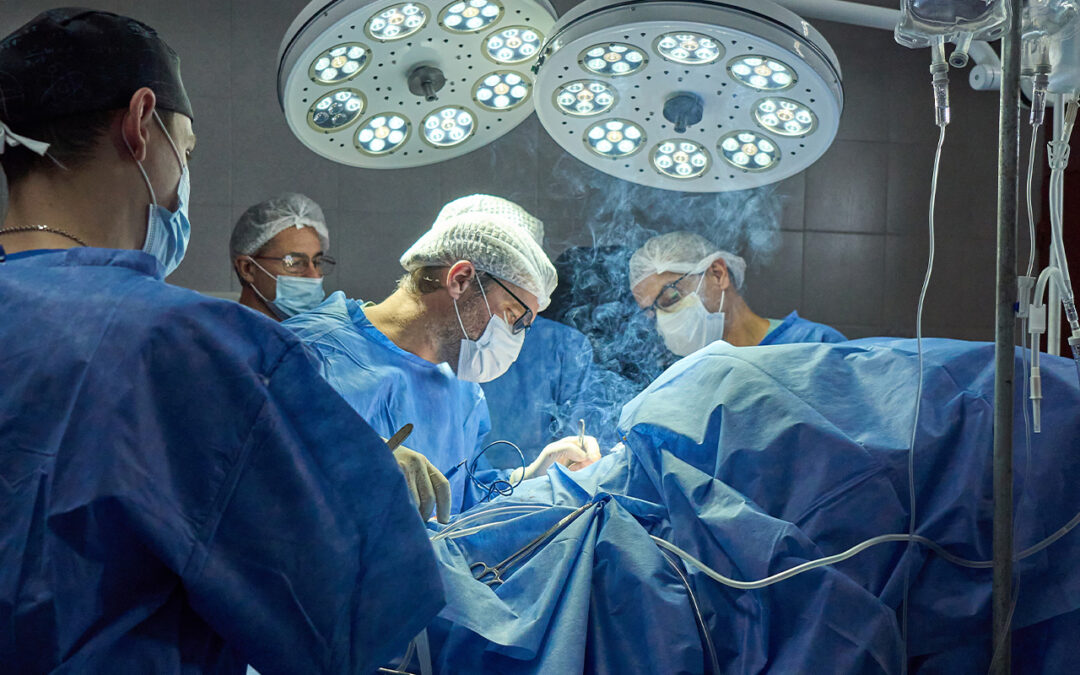
The operating room is a major contributor to these emissions, generating up to 30% of a hospital’s total waste and using up to six times more energy per square foot than other areas. This makes it critical for healthcare organizations to lead the way in “green surgery” by promoting more sustainable surgical practices.
“These numbers show that the operating room has an outsized environmental footprint, but they also reveal huge opportunities for improvement,” says Erin Kyle, DNP, RN, CNOR, NEA-BC, editor-in-chief of the Association of periOperative Registered Nurses (AORN) Guidelines for Perioperative Practice.
Minimizing Surgery’s Environmental Impact
For Daphny Peneza, DNP, RN, CNOR, CSSM, FSIEN, FAORN, perioperative services manager, neurosurgery and neurointerventional ORs at Vanderbilt University Medical Center, green surgery represents a commitment to minimizing environmental impact while upholding the highest standards of patient safety.
“As a healthcare leader, it means integrating eco-conscious practices into every aspect of perioperative care – from streamlining supply decisions to encouraging waste reduction and segregation without compromising clinical outcomes,” says Peneza. “These practices must be embraced and carried forward by every perioperative team member.”
Throughout her career, Peneza has witnessed firsthand how resource-intensive the operating room can be. “This underscores the urgency of adopting sustainable practices in perioperative settings,” she says.
Kyle believes that green surgery equates to making the OR as environmentally responsible as possible while providing optimal patient care. “Sustainable surgery is about examining everything we do in perioperative care – from the supplies we use to how we handle waste and energy – and finding ways to reduce waste, conserve resources and minimize exposure to harmful chemicals.”
“The operating room is one of the most resource-heavy areas in the hospital,” says Catarina Paulson, the head of corporate sustainability at Getinge. “Sustainable practices help hospitals do more with less by cutting waste, reducing costs and increasing efficiency.”
A Mixed Bag for Sustainability
It’s a mixed bag for healthcare organizations when it comes to improving surgical sustainability. “Progress is being made, but it remains inconsistent,” says Peneza. “Some hospitals and ASCs have embraced sustainable practices like recycling and reprocessing programs while others are in the early stages of adoption.”
Leadership commitment and staff education are critical to moving from isolated sustainability initiatives to system-wide culture change, adds Peneza.
Kyle agrees: “Overall we’re making progress, but there’s plenty of room to improve. Smaller organizations especially may not have started green initiatives due to limited resources or lack of a champion. The good news is that the trend is positive – even those that are behind the curve are starting to talk about sustainability and take first steps. Awareness is up and momentum is building.”
For example, Kyle says that many hospitals now have green OR committees and sustainability teams that include surgeons, anesthesiologists and nurses. “There’s more top-down support, too,” she says. “Some health systems have hired sustainability officers or set climate goals that push the OR to act.”
Paulson says she’s seeing increasing awareness of how product choices can affect resource consumption. “There’s a growing openness to collaborating on solutions to reduce the environmental impact of surgery,” she says. “While sustainable surgery is complex, optimizing how products are used and how waste is handled can make a significant difference.”
Waste Handling and Management
According to data from the World Health Organization (WHO), most of the waste generated in healthcare settings is nonhazardous. “Therefore, separating nonhazardous waste from hazardous waste can reduce costs associated with waste disposal and decrease the risk of exposure for healthcare workers and the environment,” stated Zach Swartz, MHI, BSN, RN, EBP-C, CNOR, a perioperative practice specialist with AORN, in “Waste Management,” an article that published in a recent issue of the AORN Journal.
“Make sure everyone knows what goes in regular trash versus red biohazard waste bags,” says Kyle. “Only true infectious material should go in red biohazard bags; nearly everything else, including packaging and paper, can go in normal trash or recycling.”
Peneza agrees: “Segregating waste streams correctly, reducing red-bag waste and recycling packaging materials are essential practices. In my experience, ensuring the appropriate number of bins for proper segregation and updating garbage bag kits have helped drive strong team compliance and accountability.”
According to Swartz, medical waste should be sorted according to the following types:
- Nonhazardous waste: This is waste that does not pose a physical, radioactive, biological or chemical threat to human or environmental health. Common examples are packaging, paper and food waste, which can be disposed of in a landfill or waste disposal facility
- Regulated medical waste: This is waste that is contaminated with blood, body fluids and other potentially infectious materials. It requires specific treatment and disposal to avoid posing a risk to personnel when it is compressed. Common examples include sharps, batteries, radiopaque sponges, dressings from infected wounds, and pharmaceutical and pathological waste.
- Hazardous waste: This is noninfectious waste that may be harmful and requires specific disposal, treatment and storage practices to reduce the potential for exposure. Hazardous waste may be ignitable, corrosive, toxic or highly reactive.
“Perioperative leaders should be aware of current local and state regulations for medical waste management practices,” stated Swartz in the article. “The most stringent applicable laws and regulations must be followed according to waste categories, transportation regulations and methods for disposal.”
Swartz recommended that an interdisciplinary team establish and maintain a perioperative waste management program that includes oversight of all waste management practices. “This will help reduce the risk of exposure to regulated and hazardous medical waste,” he wrote.
Benefits of Surgical Sustainability
Surgical sustainability can greatly benefit both healthcare organizations and patients. “Patients benefit from safer, more efficient care environments while hospitals and ASCs benefit from cost savings, supply stability and improved efficiency,” says Peneza. “Communities also benefit from reduced environmental burdens and better alignment with public health priorities.”
Paulson calls sustainable surgery a “triple win. Getinge believes that sustainable surgery leads to better outcomes for patients through fewer complications, smarter economics for hospitals with reduced costs and efficient workflows, and stronger public health through improved environmental impact.”
Adds Kyle: “Patients appreciate knowing their care is environmentally responsible – it gives them greater peace of mind. Sustainability also enhances a facility’s public image as a responsible, forward-thinking organization. Being known as a ‘green’ hospital can attract eco-conscious patients and staff.”
Here are some of Kyle’s top tips for effective surgical sustainability:
- Open only items that are needed instead of opening every item ‘just in case.’ “Also regularly update surgeons’ preference cards and custom packs to remove items that usually go unused,” says Kyle. “This prevents a lot of waste up front and saves money on supplies.”
- Set up recycling for clean materials such as paper, cardboard and plastics so they don’t end up in red biohazard waste bags or the regular trash. “This simple habit greatly reduces costly and polluting red-bag waste,” says Kyle.
- Save energy by turning off lights, monitors and equipment when the OR isn’t in use. Also consider using HVAC setbacks that can lower the air exchange rate, adjusting the thermostat at night or between cases to save energy, and switching to LED lighting and other energy-efficient equipment. “These simple steps can significantly cut energy use and lower costs without affecting patient care,” says Kyle.
- Adopt low-impact anesthesia practices. According to Kyle, some anesthetic gases are extremely potent greenhouse agents. For example, a single bottle of desflurane has the warming effect of roughly 2,000-4,000 pounds of CO₂. “So, avoid these anesthetic gases whenever possible and use low fresh-gas flow techniques to minimize waste gas,” she says.
“Many hospitals have made these changes and seen their anesthesia-related emissions plummet, which is a big win for the environment with no downside for patient care,” adds Kyle. - Sort medical waste properly. Studies have shown that over half of what gets thrown in red biohazard waste bags could be handled as normal trash or recycled with proper sorting. “Since red bag waste is costly and energy-intensive to treat, proper sorting lowers both environmental impact and cost,” says Kyle.
- Reprocess single-use devices. This can yield about a 50% cost savings per item. “Many ORs have saved hundreds of thousands of dollars per year through reprocessing and by switching to reusable items while keeping tons of material out of landfills in the process,” says Kyle.
Renewable Energy Transition
Paulson believes that sustainable surgery optimizes resources at every stage of the patient pathway. “This ranges from smart technology that maximizes operating room efficiency to advanced sterile reprocessing that minimizes the risk of infection while reducing consumption of detergents, water and energy,” she says.
“Because sterilization is essential in surgical care, transitioning to renewable energy sources to power these processes can significantly reduce carbon emissions,” says Paulson. “These practices improve patient care and reduce surgery’s environmental footprint while also lowering costs.”
AORN has released a position statement on environmental responsibility saying healthcare professionals have an ethical duty to protect patient health by reducing the environmental impact. The position statement offers principles and examples of sustainable perioperative practices to serve as foundational guidance.
“AORN’s stance (and my view) is that every facility should integrate environmental responsibility into perioperative practice as part of good patient care,” says Kyle. “We’re getting closer to that ideal, but we’re not there yet across the board.”
“As perioperative professionals, we should act as stewards of the environment by weaving sustainability into every step of perioperative practice so that we ‘do no harm’ not only to our patients, but also to our communities and our planet,” adds Kyle. “Ultimately, caring for the environment goes hand-in-hand with caring for our patients.”
Peneza believes that sustainable surgery isn’t a fad or trend.
“It’s a responsibility I hold deeply as a nurse and healthcare leader,” she says. “I am committed to advancing efficient perioperative and nursing practices that protect patients, strengthen team collaboration and safeguard our communities.”
Environmental conservation and health are inseparable, Peneza adds. “Therefore, we must give our perioperative spaces a fighting chance to embody this cause. The time to act is now.”
“Perioperative professionals are problem-solvers and patient advocates by nature so extending that advocacy to include the environment just makes sense,” says Kyle. “We’re proving that we can care for patients and the world we all live in, which is something we can all be proud of.”